
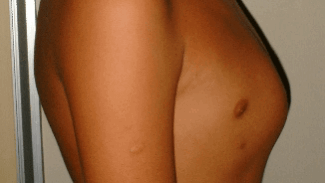
If you have noticed your child's chest becoming more prominent, it is completely understandable to have concerns. The reassuring news is that pectus carinatum is not a dangerous condition in itself, and in many cases it can be managed very effectively, particularly when identified during the adolescent growth years. For some children, the main concern is cosmetic and relates to confidence and body image. For others, there may be associated symptoms or underlying conditions that benefit from specialist assessment. Dr Giardini regularly sees children and teenagers with pectus carinatum and can determine whether further investigation is needed and guide you towards the right management pathway.
Pectus carinatum is a chest wall deformity in which the breastbone (sternum) is pushed forward, giving the front of the chest a prominent or bowed appearance. It is sometimes called "pigeon chest" because the shape resembles the chest of a bird. The condition is caused by an overgrowth of the cartilage that connects the ribs to the sternum, which pushes the breastbone outward beyond the normal contour of the chest wall. In some children, areas of the ribs alongside the prominence may appear depressed or sunken inward, which can make the central protrusion look more noticeable.

Pectus carinatum can affect both sides of the chest equally (symmetric type) or be more pronounced on one side than the other (asymmetric type). It is estimated to affect around 1 in 1,000 to 1 in 1,500 children and is approximately four times more common in boys than girls. Although the condition is present from birth, it is often not noticeable in younger children and typically becomes more apparent during the growth spurt of adolescence. It is unusual for pectus carinatum to be a significant concern before the age of 10 or 11.
The exact cause is not fully understood, but the condition is thought to result from a disproportionate overgrowth of the costal cartilages relative to the rest of the chest wall during periods of rapid growth. There is a recognised genetic component: around 25% of children with pectus carinatum have another family member with a chest wall deformity.
Pectus carinatum can occur as an isolated finding in an otherwise healthy child, which is the case for the majority. However, it can also be seen in association with certain connective tissue and genetic conditions, including Marfan syndrome, Loeys-Dietz syndrome, Ehlers-Danlos syndrome, Noonan syndrome, Turner syndrome, Down syndrome (trisomy 21), Edwards syndrome (trisomy 18), homocystinuria and osteogenesis imperfecta. It can also occur alongside scoliosis. If Dr Giardini suspects that a connective tissue disorder may be present, further assessment including genetic testing can be arranged.
Many children with pectus carinatum have no physical symptoms at all, and the only concern is the appearance of the chest. However, some children do experience symptoms, particularly those with more pronounced or asymmetric deformities.
Physical symptoms may include shortness of breath during exercise, chest pain or a feeling of tightness across the chest, a faster heart rate than expected during activity, and tiring more easily than peers during sport or exercise. These symptoms are thought to arise because the abnormal chest wall can be more rigid than normal, requiring greater effort to expand the ribcage during breathing. In asymmetric cases, the uneven pull of the chest wall muscles can cause discomfort on one side.
For many children and teenagers, the most significant impact of pectus carinatum is not physical but psychological. The visible chest prominence can affect confidence and body image, leading some young people to avoid activities where their chest is visible, such as swimming, changing for sport, or going to the beach. This can have a meaningful effect on social participation and self-esteem during a formative period of development. Early assessment and, where appropriate, treatment can make a real difference, both physically and psychologically.
🟢 Usually not concerning
🟡 Worth review
🔴 Seek assessment
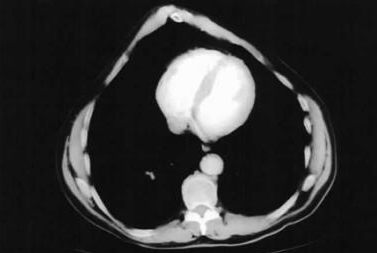
This is an important reason why children with pectus carinatum benefit from a cardiac assessment. Some children with the condition have mitral valve prolapse, where the mitral valve (the inlet valve to the left ventricle) has a slightly floppy appearance on echocardiography. In most cases, the mitral valve continues to function well, and any associated leakage is minor and of no clinical significance.
A smaller number of children, particularly those with underlying connective tissue conditions such as Marfan syndrome, Loeys-Dietz syndrome or Ehlers-Danlos syndrome, may have more significant cardiac findings. These can include enlargement of the aorta (the main artery leaving the heart), which requires monitoring over time. Dr Giardini will perform an echocardiogram to assess the heart valves, the aorta and overall heart function, and will advise on whether ongoing cardiac follow-up is needed. For the majority of children with isolated pectus carinatum and no connective tissue disorder, the heart is entirely normal.
The diagnosis is made clinically by examining the chest. In most cases, the appearance is characteristic and the diagnosis is straightforward. Dr Giardini will also assess the symmetry of the deformity, check for any features that might suggest an underlying genetic condition (such as unusually tall stature, hypermobile joints or a family history of connective tissue problems), and perform a cardiac examination.
A key part of the assessment, particularly when bracing is being considered, is evaluating the flexibility of the chest wall. This can be done with a dynamic compression test, in which gentle manual pressure is applied to the sternum to see how easily the prominence can be corrected. A flexible chest wall responds well to bracing, while a rigid one may be less likely to improve without surgery. Published data suggest that patients with a lower pressure of initial correction have better outcomes with bracing and are less likely to need surgical intervention.
Further investigations may include an echocardiogram to assess the heart, a CT or MRI scan of the chest to evaluate the bony and cartilaginous structures in detail (particularly if surgery is being considered), lung function testing to measure how the chest wall deformity is affecting breathing, and genetic testing if a connective tissue disorder is suspected.
Treatment for pectus carinatum is usually guided by symptoms, severity and how the chest shape is affecting the child. In most cases, the first-line approach is external bracing, which gently remodels the chest over time. This works best during adolescence, when the chest wall is still flexible, and relies on consistent wear for several hours each day to achieve good results. Many children are treated primarily for cosmetic reasons or concerns about confidence, although some may also report mild discomfort or reduced exercise tolerance. In situations where the deformity is more pronounced, bracing is not suitable, or results are suboptimal, surgical options can be considered, but this is less common and tailored to the individual child.
Treatment depends on the severity of the deformity, the presence of symptoms, and how the chest shape is affecting the child's quality of life.
Observation is appropriate for children with a mild prominence who have no symptoms and are not troubled by the appearance. These children do not require any active treatment but should be monitored during adolescence, as the deformity may become more noticeable during the growth spurt.
External bracing is the standard first-line treatment for pectus carinatum and has been shown to achieve excellent results in the majority of cases. The brace is a lightweight, adjustable device worn over the chest that applies gentle, sustained pressure to the prominent area, gradually remodelling the chest wall into a more normal shape. Modern dynamic compression braces can measure and adjust the pressure applied, which improves comfort and compliance.
Bracing works best during adolescence, when the chest wall cartilage is still flexible and responsive to remodelling. The ideal age to begin is typically between 11 and 14 years, although treatment can be effective outside this range. Most children are asked to wear the brace for a minimum of 12 hours per day, and many bracing protocols recommend wearing it as much as possible, including overnight. The correction phase usually takes six months to a year, after which a maintenance phase of nighttime wear continues until skeletal growth is complete to reduce the risk of recurrence. Published series report success rates of around 84% to 88% in compliant patients, and studies have shown significant improvements in self-esteem after bracing.
There can be some initial discomfort or pressure when the brace is first fitted, particularly in the first few weeks, but most children adapt quickly. The brace can usually be removed for sport, showering and special occasions. Consistent wear is the single most important factor in achieving a good result.
Surgery is reserved for cases where bracing has not been successful, where the chest wall is too rigid to respond to compression, or where the deformity is particularly severe or unusual in its anatomy. The most common surgical approach involves removing the overgrown cartilage segments and reshaping the chest wall. In some cases, a temporary metal bar (similar to the Nuss bar used in pectus excavatum) is placed behind the sternum to hold the chest in the corrected position. This bar is typically removed after one to two years. Surgery produces good results, and most children and young people who undergo successful repair go on to lead a normal life with no lasting heart or lung problems.
The outlook for children with pectus carinatum is very reassuring. The condition itself is not dangerous, and the large majority of children who receive treatment, whether through bracing or surgery, achieve a good cosmetic and functional result. Children who complete bracing properly and continue with a maintenance phase until skeletal maturity typically have durable corrections with a low rate of recurrence. Those who require surgery also do very well.
For children with an associated connective tissue disorder, Dr Giardini will arrange appropriate long-term cardiac follow-up to monitor the heart valves and aorta. For the majority of children with isolated pectus carinatum and a normal heart, no ongoing cardiac follow-up is needed after the initial assessment.
If you are concerned about your child's chest shape, or if pectus carinatum has already been diagnosed and you would like a cardiac assessment, please do not hesitate to contact Dr Giardini's team to arrange an appointment.
Mild variations in chest shape are common, particularly during growth. If the breastbone looks clearly prominent or is becoming more noticeable over time, it is worth having it assessed to confirm whether this is pectus carinatum or a normal variant.
It can be assessed at any age, but the most useful time is around the early teenage years, when growth accelerates and bracing treatment is most effective. A cardiac assessment with Dr Giardini can be performed at any stage if there are concerns about the heart.
Unlike some other developmental findings, pectus carinatum does not usually improve on its own once it becomes noticeable. It may become more prominent during the adolescent growth spurt, which is why monitoring and early assessment are important.
The active correction phase typically takes six months to a year, followed by a maintenance phase of nighttime wear until growth is complete. Most children begin to see visible improvement within the first few months.
There can be some initial pressure and discomfort, particularly in the first few weeks, but most children adapt quickly. Modern braces are lightweight and adjustable, and can be removed for sport and showering.
If bracing is completed properly, including the maintenance phase, the results are usually stable and durable. Stopping treatment too early or wearing the brace inconsistently can reduce effectiveness and increase the risk of the prominence returning.
Yes. Some children develop compensatory posture changes, such as rounding of the shoulders, partly because of the chest shape and partly because of self-consciousness. Posture exercises can be a helpful part of overall management alongside bracing.
Exercise alone will not correct the chest shape, but it can improve posture, chest wall flexibility, cardiovascular fitness and confidence. Strengthening and breathing exercises are often recommended alongside bracing.
In most children, pectus carinatum occurs on its own and the heart is normal. However, if there are features suggestive of a connective tissue condition, such as unusually tall stature, very flexible joints, or a family history, further cardiac and genetic assessment is recommended. Dr Giardini can advise on whether this applies to your child.
If the chest shape is becoming more noticeable, causing symptoms, or affecting your child's confidence, it is a good time to seek assessment. Early review allows you to understand whether simple monitoring is sufficient or whether bracing would be beneficial, and ensures that any cardiac associations are checked.
Author: Dr. Alessandro Giardini, MD, PhD
Written 03/04/2026