
POTS is a syndrome (a combination of different symptoms) caused by a malfunction of the autonomic nervous system. The autonomic nervous system is a complicated network of nerves that controls some vital bodily functions and which works in an automatic mode out of our voluntary control. For example when we stand up quickly, we would all experience a slight drop of our blood pressure due largely to the effect of gravity and the body will have to enact some compensatory manoeuvres to re-establish a normal blood pressure. This will cause some of the body arteries and veins to shrink and the heart to start beating slightly stronger and faster. All this will happen in an automatic mode not under voluntary control.
The autonomic system controls many other systems in the body beside the heart rate and the size of the body arteries and veins. In some people the autonomic system may not work and leads to many of the symptoms observed in POTS.
.png)
Many conditions can affect the function of the autonomic system, thus producing “secondary” POTS. However, in some patients, a cause for POTS is not identified despite extensive investigation. POTS has been observed to commence after a viral infection, or an acute stress like surgery, a trauma or a vaccination. Many factors are also been associated with POTS and these include: physical deconditioning (being very unfit), excessive function of the adrenergic system (excessive release of adrenaline by the body), norepinephrine transporter deficiency, joint hyper mobility syndrome (Elhers-Danlos type III), chronic fatigue syndrome, mast cell activation and several autoimmune conditions.
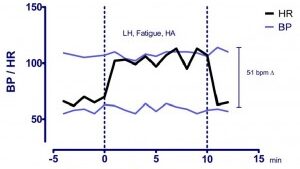
To be diagnosed with POTS children and adults have to have a combination of symptoms (not necessarily all symptoms) which occur when they are in the upright position (generally when standing) which improve (even partly) or resolve when lying down. Besides the typical symptoms, it is necessary to document an abnormal function of the component of the autonomic system that controls heart rate. In practical terms this is done by measuring the change in heart rate observed from lying down to standing up. A sustained increase in heart rate of >40 beats minute in the 10 minutes following standing is considered diagnostic in children. Blood pressure can drop while standing in patients with POTS even that is not usually the case. This test which is called an active standing test can be performed as an outpatient test.
Additional tests are required to ensure that the symptoms are not due to a cardiac or neurologic problem as many cardiac or neurologic conditions can produce very similar symptoms to POTS.
Excluding a cardiac cause for the symptoms (an arrhythmia or a structural heart problem) generally requires seeing a cardiologist with expertise in POTS as well as undertaking an electrocardiogram (ECG) and an echocardiogram. In some instances further tests may be required (24 hour ECG monitoring, active standing test, head up tilt test, cardiac MRI). Additionally blood tests will also be required at the time of the assessment.
The symptoms of POTS are numerous and can be vary disabling. This is particularly true as most of the usual cardiology investigations and tests performed in children and adults with POTS will be usually reported as normal despite patients objectively reporting the heart rate as being excessively high and the heart pounding (palpitations). Additionally many physicians are unaware of POTS.
The most common symptoms noted in POTS are:
Some triggers are known to worsen symptoms:
The diagnosis of PoTS in children and adolescents is based on a combination of the clinical history and a documented abnormal heart rate response to standing. The key test is called an active standing test. The child lies flat for at least ten minutes while heart rate and blood pressure are recorded, and then stands up quickly and remains standing for a further ten minutes. A sustained increase in heart rate of 40 beats per minute or more within those ten minutes, in the absence of a significant drop in blood pressure, is considered diagnostic. An overall and persistent increase in the heart rate above 120 beats/minute in the 10 minutes of standing is also an accepted criteria for the diagnosis. This test is simple, painless, and can be performed in the outpatient clinic. In cases where the diagnosis remains uncertain, a head-up tilt table test provides a more controlled assessment: the child is secured to a table that is tilted to a near-upright position while heart rate, blood pressure, and symptoms are monitored continuously. An ECG is essential to rule out arrhythmias or electrical abnormalities that might mimic PoTS symptoms. An echocardiogram is performed when there is any clinical suspicion of structural heart disease, an abnormal cardiac examination, or a relevant family history. Blood tests are used to exclude contributing conditions such as thyroid dysfunction, iron deficiency anaemia, and vitamin D deficiency. In selected cases, a 24-hour Holter monitor or a cardiopulmonary exercise test may be added to complete the picture. Dr Giardini performs the active standing test, ECG, and echocardiogram together as part of a single appointment, allowing a clear diagnosis and management plan to be established on the same day.
Many of the symptoms of POTS can improved with a multidisciplinary approach which includes lifestyle changes, counter maneuvers, physiotherapy/exercise and medications. Medications include those that slow down the excessive increase of heart rate (ivabradine or beta-receptors blockers), those that increase blood pressure (midodrine) and those which expand blood volume (fluidrocortisone). Medications are generally used to get children well enough to be able to start a physiotherapy/rehabilitation program. The majority of children who develop POTS as adolescents will not have symptoms by the time they will be young adults.
Author: Dr. Alessandro Giardini, MD, PhD
Written 03/04/2026