When a parent is told that their child has an anomalous coronary artery, the reaction is often a mixture of confusion and fear. The term is unfamiliar, and the potential link to sudden cardiac death in young athletes understandably causes alarm. Yet the picture is considerably more nuanced than the headline suggests: the majority of coronary artery anomalies are entirely benign, and even the small number that carry genuine risk can be identified and managed effectively with expert assessment.
This page explains what coronary artery anomalies are, how they differ from one another, what the risk profile of each looks like, how diagnosis works, and what treatment and follow-up involve. Dr. Alessandro Giardini’s specialist background in complex congenital heart conditions and exercise physiology means that families dealing with this diagnosis can access expert, personalised assessment in London.
What Are Coronary Artery Anomalies?
The coronary arteries are the blood vessels that supply the heart muscle with oxygen and nutrients. In a normal heart, two coronary arteries arise from the aorta (the main blood vessel leaving the heart): the left coronary artery, which supplies the front and left side of the heart muscle, and the right coronary artery, which supplies the back and right side. Both follow predictable pathways around the heart.
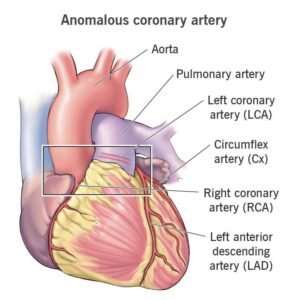
A coronary artery anomaly occurs when one or more of these arteries develops abnormally during foetal development. The anomaly may affect where the artery originates, which vessel it arises from, the path it takes through the heart and surrounding structures, or how it ends.
Coronary artery anomalies occur in less than one per cent of the general population, making them rare but not uncommon. Crucially, more than 80 per cent of all coronary artery anomalies are benign variants that cause no alteration in coronary blood supply and carry no serious clinical consequences. A smaller group are potentially serious and require specialist evaluation. A very small minority are genuinely high-risk and need treatment.
Types of Coronary Artery Anomalies
Understanding the different types helps parents make sense of what they are told and ask the right questions.
Anomalous Aortic Origin of a Coronary Artery (AAOCA)
In this group, one coronary artery arises from the wrong part of the aorta. The two most important subtypes are:
Anomalous aortic origin of the left coronary artery (AAOLCA): The left coronary artery arises from the right coronary sinus (the wrong side of the aorta) and must cross between the aorta and the pulmonary artery to reach the left side of the heart. This interarterial course can compress the artery, reducing blood flow during exertion. AAOLCA carries the higher risk among the two subtypes and is the more common cause of sudden cardiac death associated with coronary anomalies in young people. At times, as the left coronary artery originates is a slanted fashion, the initial part of the left coronary artery may run within the wall (intramural) of the aorta. In this situation the ostium (origin of the coronary artery) may also be “slit like” instead of circular. This can further compromise the flow during exercise.
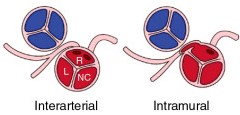
Anomalous aortic origin of the right coronary artery (AAORCA): The right coronary artery arises from the left coronary sinus and takes an interarterial course. This is generally considered lower risk than AAOLCA, though the risk is not zero and management decisions in asymptomatic children represent one of the genuinely uncertain areas in paediatric cardiology. Not every child with AAORCA needs surgery, and the decision requires careful individual assessment. In this variant the origin of the artery can be intramural as well as seen for the AAOLCA.
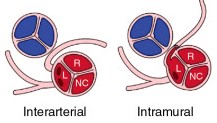
The risk with both subtypes relates to the course the anomalous artery takes between the aorta and pulmonary artery as well as presence of an intramural course. During exercise, when both these vessels enlarge and pulsate, the coronary artery running between them can be compressed. This reduces blood supply to the heart muscle at precisely the moment demand is greatest.
Anomalous Left Coronary Artery from the Pulmonary Artery (ALCAPA)
ALCAPA is the most urgent of all coronary artery anomalies. Instead of arising from the aorta, the left coronary artery originates from the pulmonary artery. The pulmonary artery carries oxygen-poor blood, so the left coronary artery delivers deoxygenated blood to the heart muscle rather than the oxygen-rich blood it needs. The result is progressive ischaemia (oxygen starvation) of the heart muscle, leading to heart failure, potentially to myocardial infarction (a heart attack in a baby), and, if untreated, to death.
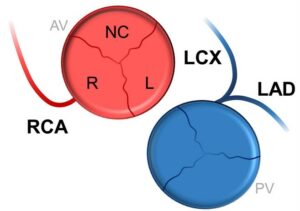
A phenomenon called coronary steal worsens the situation: because pressure in the pulmonary artery is lower than in the aorta, blood from the left coronary actually flows backwards into the pulmonary artery rather than forward into the heart muscle. This steals blood from the heart at a time when it is already severely deprived.
ALCAPA affects approximately one in 300,000 babies. Without surgery, the mortality rate in symptomatic infants exceeds 90 per cent. With timely surgery, most children do very well and go on to live normal lives.
Myocardial Bridge
A myocardial bridge occurs when a segment of a coronary artery (most commonly the left anterior descending artery) runs through the heart muscle itself rather than along the surface of the heart. During each heartbeat, the muscle contracts and squeezes the segment of artery tunnelled inside it. In most people this causes no problem at all, and myocardial bridges are generally considered a benign anatomical variant.
In a minority of cases, a deep or long bridge can cause symptoms during exercise, including chest pain and, very rarely, arrhythmias. Assessment with stress imaging and occasionally fractional flow reserve measurement (a catheter-based test that assesses pressure across the bridge during peak flow) helps identify the small group who need treatment.
Other Coronary Artery Anomalies
Several other variants exist, including coronary artery fistulae (abnormal connections between a coronary artery and a heart chamber or vessel), coronary artery atresia (absence or underdevelopment of a coronary artery), and a range of origin and course anomalies that account for the benign majority. Most of these produce no symptoms and need only routine monitoring.
Kawasaki Disease and Acquired Coronary Artery Anomalies
Not all coronary artery abnormalities in children are present from birth. Kawasaki disease, an inflammatory condition primarily affecting young children, causes inflammation of the coronary arteries. Inadequately treated Kawasaki disease can produce coronary artery aneurysms (dilated, weakened segments of the artery) that may persist, narrow, or thrombose over time. Children with coronary artery aneurysms following Kawasaki disease need long-term specialist cardiological follow-up.
How Common Are Coronary Artery Anomalies?
Coronary artery anomalies collectively affect less than one per cent of the population. AAOCA occurs in around 0.3 to 0.6 per cent of children undergoing echocardiography, making it rare but more commonly diagnosed than it was in previous decades as echocardiography has become more widespread. ALCAPA affects approximately one in 300,000 births. Myocardial bridges are considerably more common but almost always benign.
Many coronary artery anomalies are discovered incidentally, during echocardiography arranged for an unrelated reason such as a murmur or a family history of heart disease. Others present through symptoms, and a small number present through a serious event.
What Symptoms Should Parents Look For?
Symptoms depend on the type of anomaly and the child’s age.
In infants with ALCAPA, symptoms typically appear within the first two to three months of life, as pulmonary arterial pressure falls and the coronary steal phenomenon develops. Signs include irritability and crying that seems to worsen during feeding (because feeding is exercise for a baby), pallor, sweating, difficulty feeding, and poor weight gain. Some babies have breathing difficulties. An enlarged heart and heart failure develop as the condition progresses.
In older children and teenagers with AAOCA or other anomalies, symptoms are more likely to occur during exercise. Chest pain or tightness during sport, unexplained fainting or near-fainting during physical activity, palpitations, and reduced exercise tolerance all warrant cardiac evaluation. Crucially, in some children with high-risk anomalies, sudden cardiac arrest during exercise is the first manifestation, with no prior warning symptoms. This possibility, while uncommon, is the reason that unexplained exertional symptoms always need assessment in children. This is also the reason why cardiac screening of young athletes is so important.
Some children have no symptoms at all. The anomaly is found during investigation of an unrelated concern, or during family screening.
How Are Coronary Artery Anomalies Diagnosed?
Diagnosis in most children involves a combination of the investigations below.
Echocardiogram
The echocardiogram is the first-line investigation. A skilled operator can visualise the origins of both coronary arteries on echocardiography and identify anomalous origins in many cases. The test also assesses heart function, which is critical in ALCAPA where ventricular dysfunction may already be present at the time of diagnosis.
Electrocardiogram (ECG)
The ECG provides information about heart rhythm and can show signs of myocardial ischaemia or injury. In ALCAPA, the ECG may show patterns consistent with myocardial infarction. A normal ECG does not exclude a significant coronary anomaly.
Cardiac CT Angiography
CT angiography provides the most detailed anatomical definition of coronary artery origins and courses, with high spatial resolution that clearly demonstrates interarterial pathways. It remains the gold standard for defining coronary anatomy before surgical planning. CT involves radiation exposure, and most centres defer CT in young children without symptoms until they are old enough for the radiation risk to be proportionate. In symptomatic children, or where echocardiography has not fully defined the anatomy, CT provides essential information.
Cardiac MRI
Cardiac MRI defines coronary anatomy without radiation, though with slightly lower spatial resolution than CT for very small coronary vessels. MRI also assesses myocardial perfusion (whether adequate blood reaches the heart muscle) and heart function. Many centres prefer MRI for follow-up imaging once anatomy has been defined by CT, to avoid cumulative radiation.
Exercise Testing
An exercise test (treadmill or bicycle ergometer) evaluates the heart’s response to progressive physical activity. It looks for ECG changes, symptoms, and arrhythmias that emerge at higher heart rates, helping to identify children in whom the anomalous coronary causes problems during exertion. Exercise testing forms a central part of risk assessment and sports clearance decisions.
Dr. Giardini’s specific expertise in exercise physiology in children with heart conditions means that exercise testing and sport-related risk assessment form a particularly well-developed part of his practice.
Cardiac Catheterisation and Fractional Flow Reserve
Cardiac catheterisation, in which a fine tube measures pressures and blood flows directly inside the heart and coronary arteries, is sometimes used when other investigations leave the functional significance of an anomaly uncertain. Fractional flow reserve (FFR) is a specialised catheter measurement that quantifies blood flow across a narrowing or bridge during maximal vasodilation, helping identify which anatomical anomalies actually produce haemodynamically significant flow reduction.
Do All Coronary Artery Anomalies Need Treatment?
No. The majority of coronary artery anomalies are benign and need only periodic monitoring. Treatment depends on the specific anatomy, presence of symptoms, findings on exercise testing, and risk assessment.
Observation and Monitoring
Children with benign anatomical variants or low-risk AAORCA without symptoms, normal exercise testing, and no evidence of ischaemia typically need regular echocardiographic follow-up and clinical review rather than intervention. As children grow and undertake more demanding physical activity, their risk profile may change, and monitoring allows reassessment at the right times.
Exercise and Sport Guidance
For higher-risk anomalies, exercise restriction reduces the risk of sudden cardiac arrest during exertion. This is a significant decision that affects a child’s life, school experience, and emotional wellbeing, and the specific guidance must come from a specialist who has reviewed all the available investigations. The goal, wherever possible, is to define a safe level of activity rather than impose blanket restrictions. With appropriate treatment, many children return to full sporting participation.
For children with lower-risk anomalies, sport participation is often possible with careful monitoring. The key is individual assessment rather than applying generic rules.
Surgery
Surgical treatment is the definitive approach for anomalies that pose genuine risk. For ALCAPA, surgery is urgent and life-saving: the aim is to establish a two-coronary-artery system by reimplanting the anomalous left coronary artery into the aorta (the most common approach) or, when direct reimplantation is not feasible, by using the Takeuchi technique (creating a tunnel within the pulmonary artery to redirect blood from the aorta to the coronary artery). With timely surgery, cardiac function typically recovers well, and most children go on to live full, active lives.
For AAOLCA, surgery (most often an unroofing procedure, which opens the wall between the anomalous coronary artery and the aorta to enlarge the ostium) is generally recommended in symptomatic children and in most children over ten years of age even without symptoms, because the risk of sudden death during the adolescent years justifies intervention. The decision about asymptomatic AAORCA is more nuanced and represents one of the areas where careful, expert discussion with the family matters most.
Reimplantation (moving the coronary artery to its correct origin on the aorta) offers anatomical normalisation for some variants, and surgeons at specialist centres have considerable experience with this approach.
Medication
Medications do not correct coronary artery anomalies. However, in children with ALCAPA awaiting surgery, medications to manage heart failure and support cardiac function form a critical part of stabilisation before the operation. Beta-blockers, diuretics, and ACE inhibitors may be used in this context.
What Is the Long-Term Outlook?
For children with benign coronary variants, the outlook is entirely normal with no long-term implications.
For AAOCA, surgical outcomes are very good for children who receive appropriate treatment. The unroofing procedure relieves the compression of the anomalous artery and in most series carries low operative risk. After surgery, most children return to normal activity including sport.
For ALCAPA, long-term outcomes after surgery depend on how much myocardial damage occurred before the diagnosis was made and the operation performed. Children who undergo surgery early in infancy, before significant heart muscle damage has accumulated, tend to have the best recovery of cardiac function. Some children repaired later in infancy have residual mild impairment of ventricular function that may improve gradually over months to years of follow-up. Mitral valve function also recovers in most children after surgery, though occasional further intervention for the mitral valve may be needed.
All children with significant coronary artery anomalies, repaired or under monitoring, need lifelong specialist cardiac follow-up. As they reach adulthood, care transfers to an adult congenital heart disease service.
When Should You Seek Specialist Advice?
Specialist assessment is important in the following situations. If your child has been diagnosed with a coronary artery anomaly of any type, specialist review helps define the anatomy precisely, assess risk, and plan management. If a child experiences chest pain or tightness during exercise, unexplained fainting during physical activity, palpitations, or markedly reduced exercise tolerance, these symptoms need cardiac evaluation and a coronary artery anomaly should be among the possibilities considered. A family history of sudden unexplained cardiac death in a young relative warrants cardiac screening of children in the family.
If your child needs sports clearance and has a known cardiac diagnosis, formal expert assessment is essential before returning to competitive or high-intensity sport.
Dr. Alessandro Giardini offers specialist assessments for children and teenagers with suspected or confirmed coronary artery anomalies at The Portland Hospital and the Harris International and Private patients Division at Great Ormond Street Hospital. His background in congenital heart disease, combined with specific expertise in exercise physiology, makes him particularly well-placed to guide sport clearance and risk assessment decisions.
Frequently Asked Questions
Are coronary artery anomalies always serious?
No. More than 80 per cent of coronary artery anomalies are benign variants that cause no problems and need only routine monitoring. A smaller group require careful risk assessment, and a minority need treatment. The key is accurate diagnosis and expert evaluation of the specific anatomy, which is why specialist assessment matters.
Can coronary artery anomalies cause sudden cardiac death in children?
Certain high-risk anomalies, particularly an anomalous left coronary artery arising from the right aortic sinus and taking an interarterial course, carry an increased risk of sudden cardiac arrest during strenuous exercise. This risk is real but uncommon, and it is the primary reason these anomalies need specialist assessment and, in many cases, surgical correction. The risk of sudden death from AAOCA between the ages of 10 and 30 years is one of the main drivers of investigation and treatment in this age group.
What is ALCAPA and how serious is it?
ALCAPA (anomalous left coronary artery from the pulmonary artery) is the most urgent coronary artery anomaly. The left coronary artery connects to the pulmonary artery instead of the aorta, meaning the heart muscle receives deoxygenated blood. Without surgery, over 90 per cent of symptomatic infants do not survive the first year. With timely surgery, most children do very well and live normal, active lives.
My child was diagnosed incidentally with a coronary artery anomaly. What should I do?
An incidental diagnosis is common, as many anomalies cause no symptoms and are found during echocardiography arranged for another reason. The next step is a careful assessment to determine the type of anomaly, its anatomical course, and its risk profile. This requires specialist evaluation that includes, in most cases, cardiac CT or MRI, exercise testing, and a detailed clinical review. Many children with incidentally found anomalies require no treatment beyond monitoring.
Can my child play sport with a coronary artery anomaly?
This depends entirely on the specific anomaly and the results of the risk assessment. Many children with benign variants or lower-risk anomalies can participate in sport, including competitive sport, with appropriate monitoring. Children with high-risk anomalies typically need treatment before returning to high-intensity activity. The goal of specialist assessment is to define what is safe for each individual child, rather than applying blanket restrictions.
What is the difference between AAOLCA and AAORCA?
AAOLCA refers to the left coronary artery arising from the right side of the aorta and taking a course between the aorta and pulmonary artery. This carries higher risk. AAORCA refers to the right coronary artery arising from the left side of the aorta and taking the same interarterial course. This carries lower (but not zero) risk. The distinction matters because management recommendations differ between the two subtypes.
How are coronary artery anomalies diagnosed?
Diagnosis typically involves a combination of echocardiogram (heart ultrasound), ECG, and cardiac CT or MRI to define the coronary anatomy precisely. Exercise testing assesses how the heart performs under physical stress. Cardiac catheterisation with fractional flow reserve measurement is occasionally used to quantify whether an anomaly actually reduces blood flow during peak exertion.
Does a myocardial bridge need treatment?
Most myocardial bridges need no treatment. They are common anatomical variants that cause no symptoms in the majority of people. Occasionally a deep or long bridge causes symptoms during exercise, in which case stress imaging and sometimes fractional flow reserve measurement help decide whether intervention is warranted. When treatment is needed, surgical unroofing of the bridge effectively relieves compression.
Will my child need surgery?
Surgery is not needed for the majority of coronary artery anomalies. For ALCAPA, surgery is always urgent and essential. For AAOLCA, surgery is usually recommended. For AAORCA without symptoms, the decision is less clear-cut and depends on detailed assessment. For benign variants and most myocardial bridges, surgery is not indicated.
When should I consider a second opinion?
A second opinion is valuable when the diagnosis is unclear, when surgery is being recommended (particularly for asymptomatic anomalies), when sport restriction significantly affects your child’s life, or when you want independent confirmation of the management plan. Dr. Giardini welcomes referrals and self-referrals from families in this situation and offers consultations at his London clinics.
Author: Dr. Alessandro Giardini, MD, PhD
Written 17/04/2026

