Quick Summary
- Dilated cardiomyopathy (DCM) means the heart muscle is enlarged and weaker than normal.
- It can occur at any age in childhood, from infancy through to adolescence.
- Causes include viral infection, genetic conditions, metabolic disorders, and autoimmune disease.
- Presentation varies with age: babies may show feeding difficulties and rapid breathing; older children may report breathlessness, fatigue, or palpitations.
- Diagnosis relies primarily on echocardiography, supported by ECG, blood tests, and other investigations.
- Treatment ranges from medication to, in severe cases, advanced cardiac support or transplant assessment.
- Outcomes vary: some children recover well; others stabilise with treatment; a smaller group require more intensive long-term management.
- Family screening is an essential part of managing inherited forms of the condition.
What Is Dilated Cardiomyopathy?
Dilated cardiomyopathy affects the heart’s main pumping chamber, usually the left ventricle. The chamber becomes enlarged and contracts less forcefully than it should. Blood then circulates less efficiently than the body demands.
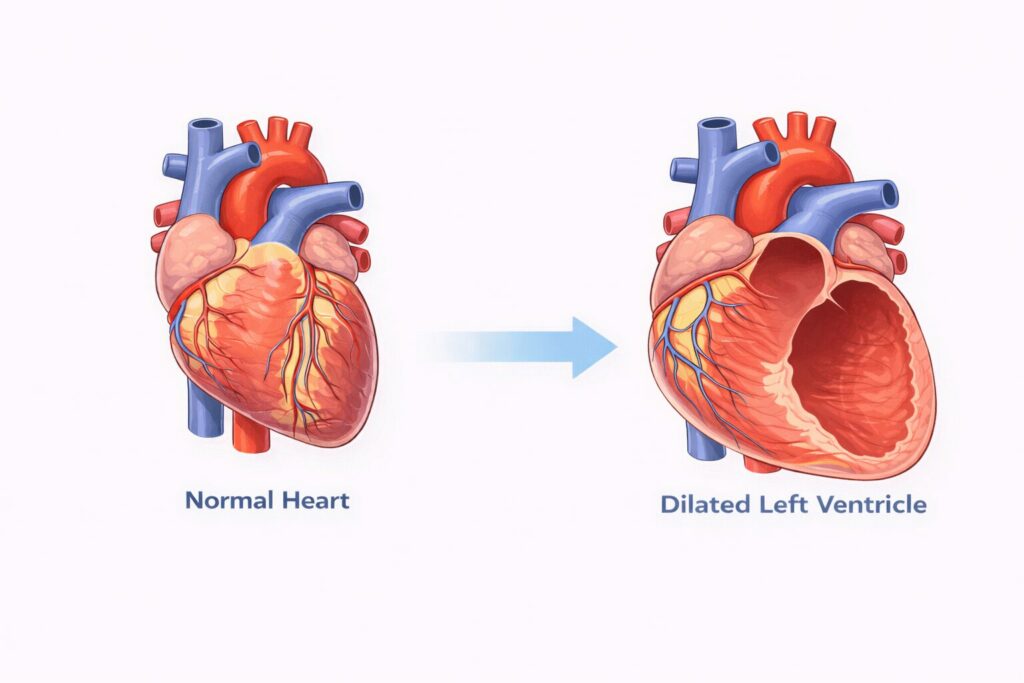
Over time, reduced pumping efficiency can cause symptoms of heart failure. Certain children have very few symptoms at the outset. The diagnosis sometimes emerges only during family screening or investigations for another problem.
Understanding the condition and what to expect is the most important first step for any family.
How Do Children with Dilated Cardiomyopathy Present?
Presentation depends very much on age. Recognising the signs at different stages allows earlier assessment and better outcomes.
Babies and Infants
In babies, symptoms can be subtle and easy to miss at first. Feeding problems or rapid breathing may seem unrelated to the heart, but they warrant attention when they persist. Parents should be alert to:
- Poor feeding or difficulty completing feeds
- Sweating during feeds
- Rapid breathing or breathlessness
- Poor weight gain despite adequate feeding
- Unusual tiredness or persistent irritability
Symptoms may develop gradually, and the underlying cardiac cause does not always declare itself clearly at the outset.
Older Children and Teenagers
Older children and teenagers can usually describe their symptoms more clearly. Common presentations include:
- Breathlessness during exercise or with normal activity
- Fatigue or reduced stamina compared with peers
- Dizziness or episodes of fainting
- Palpitations or awareness of the heartbeat
- Chest discomfort or tightness
- Swelling of the legs or abdomen in more advanced cases
Pre-symptomatic diagnosis also occurs. I sometimes encounter children where the condition surfaces only during family screening following a relative’s diagnosis.
What Causes Dilated Cardiomyopathy in Children?
Several distinct causes exist, and sometimes thorough investigation reveals no clear underlying reason.
Recognised Causes
- Viral myocarditis: infection that damages heart muscle, often following a respiratory or gastrointestinal illness
- Genetic or inherited conditions: mutations affecting heart muscle structure or function, which can run in families, including neuromuscular causes like Duchenne muscular dystrophy.
- Metabolic and syndromic conditions: rare disorders affecting energy metabolism or involving multiple organ systems
- Autoimmune disease: the immune system targeting the heart muscle
- Prior chemotherapy or other medical treatments: certain agents used in cancer treatment carry a risk of cardiac toxicity
When thorough investigation reveals no specific cause, clinicians use the term idiopathic dilated cardiomyopathy. Idiopathic DCM remains one of the more common forms seen in paediatric practice.
Does Dilated Cardiomyopathy Run in Families?
Yes, in some cases. Among children with dilated cardiomyopathy, a proportion carry an inherited genetic form of the condition. Other family members may carry the same condition, sometimes without obvious symptoms.
First-degree relatives, including parents and siblings, often warrant cardiac assessment. Evaluation typically covers an ECG and an echocardiogram. Genetic testing warrants consideration where a specific inherited cause seems likely based on the clinical picture or family history.
Family screening is one of the most important and frequently overlooked aspects of managing this condition. Identifying affected relatives early, before symptoms develop, allows appropriate monitoring and timely intervention.
When to Seek Urgent Medical Attention
Seek Emergency Help Immediately If Your Child Has:
- Severe breathlessness or difficulty breathing at rest
- Difficulty feeding with pallor or distress (in infants)
- Collapse or fainting
- Extreme tiredness or significantly reduced responsiveness
- Pale, grey, or mottled skin colour
- Rapid and unexplained worsening of any existing symptoms
Call 999 immediately. These signs can indicate that the heart is under significant strain and require prompt emergency assessment.
How Is Dilated Cardiomyopathy Diagnosed?
Making the diagnosis is usually straightforward once suspicion arises. Clinical history and examination provide essential context, and specific investigations then confirm the diagnosis and guide treatment planning.
Echocardiogram
An echocardiogram is the primary diagnostic investigation. It shows heart chamber size, wall thickness, and how well the ventricle contracts. Both the degree of enlargement and the level of functional impairment are measurable directly on this single test.
Further Investigations
Additional tests are selected based on clinical presentation and may include:
- ECG: to assess heart rhythm and look for conduction abnormalities
- Chest X-ray: to evaluate heart size and detect lung fluid retention
- Blood tests: markers of heart muscle stress, thyroid function, and metabolic screen
- Heart rhythm monitoring: Holter monitor or event recorder to detect arrhythmias
- Cardiac MRI: provides detailed structural and functional information, and can detect inflammation or scarring within the heart muscle
- Genetic testing: relevant when an inherited form seems likely, particularly with a positive family history
Not every child needs every investigation. Assessment is tailored individually, guided by age, clinical presentation, and initial test results.
What Treatment Is Needed?
Treatment depends on the severity of heart dysfunction, the underlying cause, and how the child responds clinically. Management evolves over time and requires regular review.
Medication
Most children with dilated cardiomyopathy need ongoing medication. Standard treatment typically includes medicines to support heart function, reduce cardiac workload, and manage fluid retention. Rhythm control medication addresses arrhythmias where present. Blood-thinning therapy is sometimes appropriate when pumping function is significantly impaired.
Hospital Admission and Advanced Support
Children with more severe heart failure may need hospital admission for intravenous medication, closer monitoring, and stabilisation. Intensive care support sometimes becomes necessary during acute deterioration.
Ventricular assist devices can bridge children through severe heart failure while awaiting recovery or a transplant decision. Heart transplantation addresses the needs of a small proportion of children whose function does not stabilise with maximal medical therapy. Dedicated centres conduct transplant assessment through a careful, structured process.
An Important Note on Recovery
Recovery of heart function is possible, particularly in children whose dilated cardiomyopathy followed a viral infection. Significant improvement can occur over months, and some children achieve near-complete recovery of cardiac function with appropriate treatment. Regular follow-up tracks progress carefully over time.
What Is the Outlook?
Prognosis is the question every parent asks, and it deserves an honest answer.
Dilated cardiomyopathy is a serious condition, but outcomes vary very widely. Some children recover well, particularly when a clear and treatable cause comes to light early. Others stabilise on treatment and lead active, full lives with appropriate long-term management. Certain children develop more significant heart failure and require advanced intervention over time.
Key factors include the underlying cause, the degree of dysfunction, the age at onset, and response to initial treatment. Early diagnosis and consistent specialist follow-up rank among the most important determinants of a good outcome.
What Happens Next After Diagnosis?
Parents often feel uncertain about the path ahead after receiving a new diagnosis. Knowing the typical care structure helps reduce that uncertainty.
Ongoing care usually involves:
- Regular follow-up appointments with a paediatric cardiologist
- Periodic repeat echocardiograms to monitor heart size and function over time
- Review and adjustment of medication as the clinical picture evolves
- Clear guidance on activity levels and lifestyle
- Family screening where an inherited cause is possible
- Coordination with other specialists where the cause involves additional organ systems
Follow-up frequency depends on how stable the child is clinically. Well-compensated children on treatment may attend every few months. Those with more active disease need closer monitoring.
Activity, Sport, and School
Activity guidance requires an individual approach. General statements about sport do not adequately address a condition with this range of severity.
Children with mild or recovering DCM may participate in moderate physical activity with some restrictions. Those with significant ongoing heart dysfunction generally need more conservative guidance. Competitive or high-intensity sport warrants careful assessment before resumption, and specialists advise against it until function stabilises.
Written guidance from the cardiologist helps schools and sports coaches respond appropriately, avoiding unnecessary restriction of everyday activities. Every decision about sport should involve the specialist team.
When to See a Paediatric Cardiologist in London
Cardiology review adds value across a range of situations, not only at the point of acute diagnosis. Seeking a specialist opinion is worthwhile when:
- A child has a diagnosis of dilated cardiomyopathy and the family wants a clear second opinion or coordinated care
- The diagnosis remains uncertain after initial assessment
- Symptoms such as breathlessness, fatigue, or palpitations remain unexplained
- A family history of cardiomyopathy or sudden cardiac death is present
- A relative has received a diagnosis and first-degree family members need cardiac screening
- Parents need a clear explanation of test results, treatment options, and prognosis
As a Paediatric Cardiologist in London, I regularly support families navigating a new diagnosis or seeking clarity about ongoing symptoms. My aim is to give families a clear picture of what is happening and what to expect.
Conclusion
DCM in children carries a wide range of possible outcomes. Many children improve significantly, particularly when the underlying cause receives prompt and appropriate attention. Others require careful long-term management and do well with consistent specialist support. A smaller group faces a more challenging course and may need advanced interventions.
Understanding the condition properly, recognising warning signs early, and maintaining regular specialist follow-up form the foundation of good care.
Frequently Asked Questions About Dilated Cardiomyopathy in Children
Is dilated cardiomyopathy in children rare?
Relatively uncommon, but DCM ranks among the more significant heart muscle conditions in paediatric practice.
Can children recover from dilated cardiomyopathy?
When viral myocarditis is the cause, recovery is possible and sometimes substantial. Many improve significantly, though long-term follow-up remains important for most.
Is dilated cardiomyopathy life-threatening?
It can be serious, but outcomes vary widely. Early diagnosis and appropriate treatment make a significant difference to the long-term course.
Does my child need to stop sport?
Activity guidance depends on how affected the heart is. A paediatric cardiologist should always review this before any decisions about sport are made.
Should the whole family be tested?
Screening is appropriate in certain cases. Family assessment matters most when an inherited form is suspected, and first-degree relatives often warrant an ECG and echocardiogram.
What is the most important diagnostic test?
An echocardiogram is the key test to assess heart size and pumping function. Other investigations are added based on the clinical picture.
Can dilated cardiomyopathy be caused by a virus?
Yes. Viral myocarditis is a recognised cause, and the heart muscle sometimes recovers meaningfully after the infection resolves.
Will my child need a heart transplant?
Only a small proportion of children reach this stage. Medication and regular monitoring manage the majority effectively over time.
Key Points for Parents
- Dilated cardiomyopathy means the left ventricle is enlarged and pumps less effectively than normal.
- Causes include viral infection, inherited genetic conditions, metabolic disorders, autoimmune disease, and prior chemotherapy.
- No cause is found in a significant number of children: this form is called idiopathic DCM.
- Babies present differently from older children; feeding difficulties and rapid breathing are key infant warning signs.
- Echocardiography is the central diagnostic investigation, supported by ECG, blood tests, cardiac MRI, and genetic testing where indicated.
- Medication forms the cornerstone of treatment for most children.
- Recovery of heart function is possible, especially following viral myocarditis.
- Family screening is essential when an inherited form is possible.
- Regular specialist follow-up is the foundation of long-term care.
Dr. Alessandro Giardini, MD, PhD
Written 08/04/2026

