Tetralogy of Fallot: A Complete Guide for Parents, Teenagers and Young Adults
Learning that your child has tetralogy of Fallot can be overwhelming. Whether the diagnosis came during pregnancy, shortly after birth, or later in childhood, it is natural to have many questions and to feel anxious about what lies ahead. This guide is written for parents, teenagers living with the condition, and young adults navigating life after repair. It covers everything from the basic anatomy of the condition through to surgery, recovery, long-term follow-up, and what adult life looks like — including exercise, careers, and pregnancy.
What Is Tetralogy of Fallot?
Tetralogy of Fallot (often abbreviated to TOF or “Fallot’s”) is a congenital heart condition, meaning it is present from birth. It is the most common cyanotic congenital heart defect, accounting for approximately 5 to 7 per cent of all congenital heart conditions. In the United Kingdom, roughly 1 in every 3,600 babies is born with TOF each year.
The name “tetralogy” refers to the fact that the condition involves four related structural problems within the heart. These four defects occur together because they all stem from a single underlying developmental issue: the way part of the heart forms during the early weeks of pregnancy.
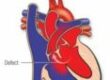
The Four Heart Defects in Tetralogy of Fallot
To understand TOF, it helps to know a little about how the heart normally works. The heart has four chambers: two upper chambers (atria) that receive blood, and two lower chambers (ventricles) that pump blood out. The right ventricle pumps blood to the lungs to pick up oxygen, and the left ventricle pumps oxygen-rich blood out to the body.
In tetralogy of Fallot, four things are different:
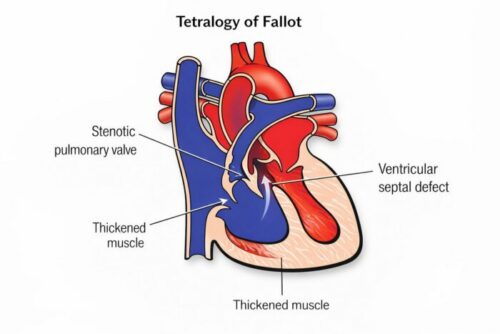
1. Ventricular Septal Defect (VSD)
There is a hole in the wall (septum) between the two lower chambers of the heart. This allows oxygen-poor blood from the right ventricle to mix with oxygen-rich blood in the left ventricle. In TOF, this hole is typically large and sits high up in the septum.
2. Pulmonary Stenosis (Right Ventricular Outflow Tract Obstruction)
The pathway from the right ventricle to the lungs is narrowed. This narrowing can occur at several levels: the muscle below the pulmonary valve (infundibular stenosis), the valve itself (valvular stenosis), or the pulmonary artery beyond the valve. This obstruction restricts the amount of blood that can reach the lungs to collect oxygen.
3. Overriding Aorta
The aorta, the large artery that carries oxygen-rich blood to the body, is positioned further to the right than normal, sitting directly over the ventricular septal defect. This means the aorta receives blood from both the right and left ventricles, rather than just the left.
4. Right Ventricular Hypertrophy
Because the right ventricle has to work harder to push blood through the narrowed pathway to the lungs, its muscular wall becomes thickened over time. This thickening is a consequence of the other three defects rather than a separate problem in its own right.
The combined effect of these four defects is that not enough blood reaches the lungs, and oxygen-poor blood is pumped out to the body. This is why some babies with TOF have a blue tinge to their skin — a sign called cyanosis.
What Causes Tetralogy of Fallot?
In most cases, the exact cause of tetralogy of Fallot is not known. It develops very early in pregnancy (during the first eight weeks) when the heart is forming, and is thought to result from a combination of genetic and environmental factors.
TOF is not caused by anything a parent did or did not do during pregnancy. It is not the result of diet, stress, exercise, or lifestyle choices.
Certain factors are associated with a slightly higher risk, including genetic conditions such as Down syndrome (trisomy 21), DiGeorge syndrome (22q11.2 deletion), maternal diabetes during pregnancy, maternal age over 40, and exposure to certain medications during early pregnancy (such as some anti-seizure drugs). However, many babies with TOF have none of these risk factors.
If your child has been diagnosed with TOF, genetic testing (particularly for 22q11.2 deletion) may be recommended, as this can have implications for other aspects of your child’s health and development.
How Is Tetralogy of Fallot Diagnosed?
Diagnosis Before Birth (Antenatal)
Tetralogy of Fallot can often be detected during routine pregnancy ultrasound scans, typically at the 18 to 20-week anomaly scan. If the sonographer suspects a heart problem, you will be referred for a specialist foetal echocardiogram (a detailed ultrasound of the baby’s heart). An antenatal diagnosis allows families to prepare and plan, and ensures the baby is born at a hospital with appropriate cardiac facilities.
Diagnosis After Birth
Some cases of TOF are not detected before birth. After delivery, the condition may be suspected if a baby appears blue (cyanotic), if a heart murmur is heard, or if oxygen levels are low on the newborn pulse oximetry screening test, a routine check now offered to all newborns in the UK.
The key investigations include pulse oximetry (measuring blood oxygen levels), echocardiography (the gold standard for confirming the diagnosis, showing the VSD, the degree of pulmonary stenosis, the position of the aorta, and the coronary artery anatomy), chest X-ray (which may show a characteristic “boot-shaped” heart), electrocardiogram (ECG) to assess the heart’s electrical activity, and in some cases cardiac MRI or CT angiography to provide additional anatomical detail before surgery.
Symptoms of Tetralogy of Fallot
The symptoms of TOF depend on the severity of the obstruction to blood flow to the lungs. They can range from very mild to severe.
In Newborns and Infants
Some babies are noticeably blue from birth (“blue babies”), while others appear pink initially and develop cyanosis gradually over the first weeks or months. Common signs include a blue or dusky colour to the skin, lips, and fingernails (especially during crying or feeding), breathlessness during feeds (babies may tire easily and take longer to feed), poor weight gain, and a heart murmur heard by a doctor.
“Tet Spells” (Hypercyanotic Spells)
One of the most frightening symptoms for parents is a “tet spell.” During a tet spell, the baby suddenly becomes very blue, breathless, and distressed. Some babies may become limp or lose consciousness briefly. Tet spells are caused by a sudden worsening of the obstruction to blood flow to the lungs and most commonly occur between 2 and 4 months of age.
If your baby has a tet spell, the immediate response is to bring the baby’s knees gently up to their chest (the “knee-chest” position). This increases blood flow to the lungs and can help to relieve the episode. You should call for emergency medical help. Tet spells are a sign that surgery may need to be brought forward.
In Older Children
In older children who have not yet had surgery (which is rare in the UK), symptoms may include turning blue during exertion, squatting after physical activity (children instinctively adopt this position because it increases blood flow to the lungs), clubbing of the fingers and toes (the fingertips become rounded and wide), and reduced exercise tolerance.
How Is Tetralogy of Fallot Treated?
All children with tetralogy of Fallot will need heart surgery. The timing and type of surgery depends on the severity of the condition and the individual child.
Complete Surgical Repair
The definitive treatment is open-heart surgery to repair all four defects. This is known as a “complete repair” or “total correction.” In most UK centres, complete repair is performed between 3 and 6 months of age, though timing can vary.
During the operation, the surgeon closes the ventricular septal defect using a patch (usually made from Gore-Tex or the child’s own pericardium), widens the narrowed right ventricular outflow tract and pulmonary valve (this may involve removing obstructing muscle bundles, cutting open the narrowed valve, or placing a patch across the outflow tract known as a “transannular patch”), and separates the mixed blood flow so that oxygen-poor blood goes to the lungs and oxygen-rich blood goes to the body.
The surgery is performed under general anaesthesia using cardiopulmonary bypass (a heart-lung machine). It typically takes 3 to 5 hours. In experienced UK centres, the surgical success rate is excellent, with operative survival rates exceeding 99 per cent.
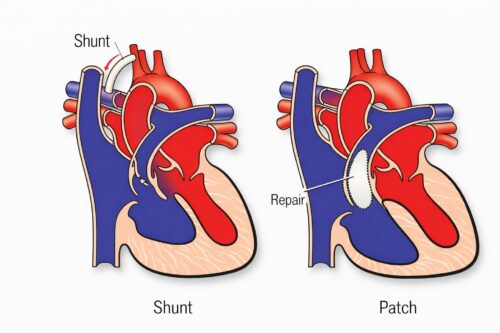
Palliative (Temporary) Surgery: The BT Shunt
If a baby is very small, very blue, or has anatomy that makes early complete repair challenging, a temporary procedure called a modified Blalock-Taussig (BT) shunt may be performed first. This involves placing a small tube (shunt) between one of the arteries to the arm and the pulmonary artery, creating an additional pathway for blood to reach the lungs. This improves oxygen levels and allows the baby to grow until complete repair can be safely performed.
Catheter-Based Procedures
In some cases, catheter-based interventions may be used, either as a bridge to surgery or as part of long-term management. These include balloon dilatation of the pulmonary valve, stenting of the right ventricular outflow tract or pulmonary arteries, and in later life, transcatheter pulmonary valve replacement (see the section on adult follow-up below).
What to Expect During Your Child’s Hospital Stay
Understanding what happens during and after surgery can help parents feel more prepared.
Before Surgery
Your child will have pre-operative assessments including blood tests, echocardiography, and in some cases cardiac MRI. The surgical team will explain the procedure, the risks, and the expected recovery. You will meet the anaesthetist, surgeon, and intensive care team.
After Surgery
After the operation, your child will be taken to the paediatric cardiac intensive care unit (CICU). They will have a breathing tube (ventilator) for a period — usually hours to a day or two, chest drains to remove fluid, continuous heart monitoring, and intravenous lines for fluids and medications. Most children spend 1 to 3 days in intensive care and a further 5 to 7 days on the cardiac ward. Parents are encouraged to be at the bedside throughout, and the nursing team will support you in caring for your child during recovery.
Going Home
Before discharge, the team will ensure your child is feeding well, gaining weight, and recovering from surgery. You will be given guidance on wound care, medication, activity restrictions, and when to seek medical advice. A follow-up appointment will be arranged, typically within 4 to 6 weeks.
Recovery After Surgery
Most children recover remarkably well from TOF repair. In the weeks after surgery, you may notice increased energy and appetite, improved colour (the blue tinge resolves), and better feeding and weight gain.
The sternotomy wound (down the centre of the chest) takes approximately 6 to 8 weeks to heal fully. During this time, your child should avoid being picked up under the arms and should not be carried in positions that put pressure on the chest.
Most babies can return to normal activities gradually, and by 3 months after surgery, the majority of restrictions are lifted. Older children are usually able to return to school within 6 to 8 weeks, with a phased return to physical education agreed with the cardiac team.
Long-Term Follow-Up: Why Lifelong Cardiology Care Matters
It is important for all families to understand that while surgery repairs the structural problems, tetralogy of Fallot is a lifelong heart condition. Even after a successful repair, ongoing cardiology follow-up is essential.
Why Is Follow-Up Needed?
After repair, many patients develop pulmonary regurgitation, a leaky pulmonary valve that allows blood to flow backwards from the pulmonary artery into the right ventricle. This is especially common when a transannular patch was used. Over years and decades, this can cause the right ventricle to stretch and enlarge, which if left unaddressed may lead to reduced heart function, exercise intolerance, and heart rhythm problems.
Other long-term issues to monitor include residual or recurrent narrowing (stenosis) of the right ventricular outflow tract or pulmonary arteries, aortic root dilatation (the aorta can gradually widen over time), heart rhythm disturbances (arrhythmias). Approximately half of all adults with repaired TOF experience some form of arrhythmia, and in rare cases, heart block requiring a pacemaker.
What Does Follow-Up Involve?
In the UK, children with repaired TOF are seen regularly by their paediatric cardiologist, usually every 12 months during childhood, with investigations including echocardiography (to assess valve function and ventricle size), ECG and Holter monitoring (to check for arrhythmias), exercise testing (typically from the teenage years), and cardiac MRI. This test is increasingly regarded as the most accurate way to measure right ventricular size and function, and essential for timing pulmonary valve replacement.
As a specialist in paediatric and congenital heart disease in London, the long-term follow-up of patients with repaired tetralogy of Fallot is a core part of my practice. I work closely with families to ensure that monitoring is thorough, timely, and tailored to each individual.
Pulmonary Valve Replacement: When and How
Many people with repaired TOF will eventually need a pulmonary valve replacement. This is the most common re-intervention after TOF repair and is typically needed in the teenage years or early adulthood, though timing varies widely.
When Is Pulmonary Valve Replacement Needed?
The decision to replace the pulmonary valve is based on a combination of symptoms (breathlessness, reduced exercise capacity, palpitations), objective findings on cardiac MRI (a dilated right ventricle, declining right ventricular function), arrhythmias, and in some cases the presence of significant tricuspid regurgitation.
Current guidelines recommend intervention before the right ventricle becomes irreversibly dilated, making timely surveillance with cardiac MRI critically important.
Surgical Pulmonary Valve Replacement
Traditionally, pulmonary valve replacement has been performed as open-heart surgery, inserting a biological (tissue) valve. This remains the gold standard, with excellent outcomes and low surgical risk in experienced centres.
Transcatheter Pulmonary Valve Replacement (TPVR)
An increasingly important option is transcatheter pulmonary valve replacement, a minimally invasive procedure in which a new valve is delivered via a catheter through a vein in the leg, avoiding the need for open-heart surgery. Recent research (2024–2025) has demonstrated that TPVR achieves excellent technical success rates (above 98 per cent) with a safety profile comparable to surgical replacement. A 2025 systematic review and meta-analysis confirmed that TPVR is non-inferior to surgical valve replacement in repaired TOF patients, though long-term durability data beyond 10 years are still being collected. Not all patients are suitable for TPVR: it depends on the anatomy of the right ventricular outflow tract. Your cardiologist will advise which approach is best for your situation.
For Teenagers: Living With Repaired Tetralogy of Fallot
If you are a teenager who had TOF repair as a baby, you may not remember your surgery at all. You might feel perfectly well and wonder why you still need to see a cardiologist. This section is for you.
Why Do I Still Need Check-Ups?
Even though you feel fine, changes can happen gradually to your heart, so slowly that you might not notice any difference. Regular check-ups allow your cardiologist to detect changes early, before they cause problems. Think of it like a car service: things can wear over time even when the engine still runs.
Can I Play Sports and Exercise?
Most teenagers with repaired TOF can and should be physically active. Exercise is good for your heart. For the majority, moderate-intensity activities like running, swimming, cycling, football, dancing are safe and encouraged.
If your repair is straightforward and your heart function is good, you may be cleared for competitive sport as well. However, some individuals with significant residual problems (a very leaky valve, reduced heart function, or arrhythmias) may be advised to avoid high-intensity competitive or contact sports. Your cardiologist will give you personalised advice based on your most recent investigations.
The key message is: do not avoid exercise entirely. Inactivity carries its own risks. Stay active, stay fit, and discuss any concerns with your cardiology team.
Emotional Wellbeing
Living with a heart condition can sometimes feel isolating, especially during the teenage years. It is completely normal to feel anxious, frustrated, or different from your peers. If you are struggling, talk to your cardiac team. Many centres have psychologists or counsellors experienced in supporting young people with congenital heart disease.
Transitioning to Adult Services
At some point during your late teens or early twenties, your care will transfer from a paediatric cardiologist to an adult congenital heart disease (ACHD) specialist. This is called “transition” and it is carefully planned. You will not simply be moved: there are joint clinics and handover meetings designed to ensure continuity of care.
Tetralogy of Fallot in Adult Life
Thanks to the success of modern cardiac surgery, the vast majority of people born with TOF today will live well into adulthood. The 30-year survival after repair exceeds 95 per cent. However, TOF is a lifelong condition, and adults need ongoing specialist care.
Careers and Daily Life
Adults with repaired TOF lead full and productive lives. There are very few careers that are restricted. Some roles with very specific physical demands (such as military combat roles or commercial airline piloting) may not be open to you, but the vast majority of professions are fully accessible. Many adults with repaired TOF run businesses, work in demanding professions, travel the world, and live completely independently.
Pregnancy and Family Planning
For women with repaired tetralogy of Fallot, pregnancy is possible and often successful. The 2025 ESC Guidelines for the management of cardiovascular disease and pregnancy provide updated guidance for women with congenital heart disease.
Before becoming pregnant, it is essential to have a thorough cardiac assessment with your cardiologist. This will evaluate your heart function, valve function, arrhythmia risk, and overall fitness for pregnancy. In most cases, particularly when the repair is straightforward, the heart function is good, and there are no significant arrhythmias then the risk of pregnancy is low and outcomes are excellent.
Some women with more complex residual problems (severe pulmonary regurgitation, significant right ventricular dilatation, or arrhythmias) may need their valve replaced before pregnancy, or may require closer monitoring during pregnancy. A multidisciplinary team including an obstetrician, cardiologist, and anaesthetist will work together to plan your care.
Women taking certain cardiac medications should discuss these with their cardiologist before becoming pregnant, as some drugs need to be changed or stopped.
Men with repaired TOF can father children normally. If your child has TOF, the chance of your children having a congenital heart defect is slightly higher than the general population (approximately 3 to 5 per cent, compared with about 1 per cent overall), but the majority of your children will have completely normal hearts.
Insurance, Driving and Travel
Adults with repaired TOF are usually able to drive without restriction, provided they do not have uncontrolled arrhythmias or a defibrillator implanted (in which case specific DVLA rules apply). Travel insurance can sometimes be more expensive or complex, but specialist insurers familiar with congenital heart disease can help. You should always carry a medical summary when travelling abroad.
Frequently Asked Questions About Tetralogy of Fallot
Below are the questions that parents and young people most commonly search for, answered in plain language.
1. What is tetralogy of Fallot in simple terms?
Tetralogy of Fallot is a heart condition that babies are born with. It involves four problems with the structure of the heart that, together, mean not enough blood gets to the lungs to pick up oxygen. This can cause the baby to appear blue. It is treated with heart surgery, usually within the first six months of life, and the vast majority of children go on to live full and active lives.
2. Is tetralogy of Fallot life-threatening?
Without treatment, TOF is serious. Historically, fewer than half of untreated children survived beyond the age of 10. However, with modern surgery, outcomes are excellent. The operative survival rate in experienced UK centres exceeds 99 per cent, and long-term survival after repair is over 95 per cent at 30 years. TOF is treatable, and most children thrive after surgery.
3. What causes tetralogy of Fallot? Did I do something wrong?
No. TOF develops very early in pregnancy due to a combination of genetic and environmental factors that are largely beyond anyone’s control. It is not caused by anything a parent ate, drank, or did during pregnancy. In most cases, no specific cause is identified.
4. Will my child need more than one operation?
The initial complete repair is usually the only major surgery in childhood. However, many people with repaired TOF will need a pulmonary valve replacement later in life, typically during the late teenage years or early adulthood. Some patients may also need catheter-based procedures to address residual narrowing or other issues. Lifelong cardiology follow-up ensures that any re-intervention is planned at the optimal time.
5. Can my child play sports and be physically active?
Yes and they should. Most children with repaired TOF can participate in sports and physical activity, including school PE, swimming, cycling, and team sports. Your cardiologist will provide individualised advice based on your child’s heart function. In general, regular exercise is strongly encouraged. Only a small number of patients with significant residual problems may be advised to avoid very high-intensity competitive sport.
6. What are “tet spells” and what should I do if my baby has one?
A tet spell is a sudden episode in which the baby becomes very blue, breathless, and distressed. It is caused by a temporary worsening of the blood flow obstruction to the lungs. If it happens, bring your baby’s knees gently up to their chest and call 999 immediately. Tet spells are a sign that surgery may need to happen sooner.
7. Will my child have a normal life expectancy?
With modern surgical techniques and lifelong follow-up, most people with repaired tetralogy of Fallot can expect to live a long and full life. The 30-year survival exceeds 95 per cent, and many adults with repaired TOF are now living into their 60s, 70s, and beyond. The key is maintaining regular follow-up with a specialist in congenital heart disease to monitor for and address any late complications.
8. Is tetralogy of Fallot genetic? Could my other children have it?
TOF has a genetic component, but it is not inherited in a simple pattern. If one child has TOF, the risk of a sibling having any congenital heart defect is slightly higher than the general population, roughly 2 to 3 per cent compared with the baseline risk of approximately 1 per cent. In some cases, TOF is associated with genetic syndromes such as 22q11.2 deletion (DiGeorge syndrome), and genetic counselling may be recommended.
9. Can women with repaired tetralogy of Fallot have babies?
Yes. Many women with repaired TOF have successful pregnancies and healthy babies. The key is careful planning. Before becoming pregnant, you should have a full cardiac assessment to evaluate your heart function, valve function, and arrhythmia risk. Most women with a good repair and stable heart function are considered low to moderate risk. A specialist multidisciplinary team will monitor you throughout pregnancy to ensure the best possible outcome for you and your baby.
10. What happens when my child becomes an adult? Do they still need a heart doctor?
Yes, lifelong cardiology follow-up is essential. During the late teenage years, care will be transferred from a paediatric cardiologist to an adult congenital heart disease (ACHD) specialist through a structured transition process. Adults with repaired TOF need regular monitoring for pulmonary valve function, right ventricular size, arrhythmias, and exercise capacity. This ongoing care is what ensures excellent long-term outcomes.
Dr. Alessandro Giardini, MD, PhD
Written 31/03/2026