Being told that your child has a patent foramen ovale (a PFO) can feel alarming, particularly when it comes as an unexpected finding during a scan. The most important thing to understand from the outset is that a PFO is not a heart defect in the usual sense. It is a normal anatomical variant, present in roughly one in four people, and in the vast majority of children it requires no treatment, no medication, and no restrictions on activity whatsoever.
This page explains what a PFO is, why it is found so frequently in children, and when, in rare circumstances, it might be worth discussing further with a specialist.
What Is a Patent Foramen Ovale?
The Foramen Ovale in Normal Development
Before birth, a baby’s lungs are not in use. Instead, oxygen is delivered through the placenta, and blood circulates differently from the way it does after birth. To allow blood to flow efficiently through the fetal circulation, there is a small opening between the two upper chambers of the heart, the right and left atria, called the foramen ovale. This opening is present in every baby and is a completely normal, intentional feature of fetal heart development.
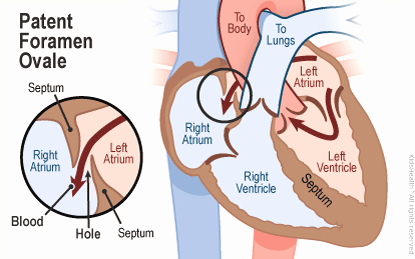
At birth, as a baby takes its first breath and the lungs begin to function, the pressure inside the heart changes. In most babies, this pressure change causes the foramen ovale to close naturally within the first few weeks or months of life. The two tissue flaps that form the opening press together and, over time, fuse shut.
When It Stays Open
In approximately one in four people, the foramen ovale does not fully seal. It remains as a small, flap-like opening that can potentially allow a tiny amount of blood to pass between the right and left atria under certain conditions. This persistent opening is what is called a patent foramen ovale.
It is worth emphasising that this is not a structural defect or a malformation. It is simply a variation in the way the heart develops, and it is one of the most common incidental findings in paediatric cardiology.
How Common Is a PFO?
Very common. Around one in four children and adults have a PFO, making it by far the most frequently identified incidental cardiac finding on echocardiogram. In most cases it is discovered entirely by chance, during an echo performed for an unrelated reason. Many people live their entire lives without ever knowing they have one.
Does a PFO Cause Symptoms?
Almost never. A PFO is not a cause of chest pain, palpitations, breathlessness, or exercise limitation in children. If a child has any of these symptoms, the PFO is almost certainly not responsible, and the symptoms deserve investigation in their own right.
This is one of the most important reassurance points for parents: finding a PFO does not explain symptoms, and it does not mean the heart is under strain or working abnormally. The heart functions normally with a PFO present.
When Might a PFO Be Relevant?
In Children: Rarely
In the paediatric context, a PFO is genuinely relevant in only a very small number of specific situations. The most significant is cryptogenic stroke, a stroke with no obvious identified cause, in a child where the PFO might theoretically have allowed a small clot to pass from the right side of the heart to the left and travel to the brain. Even here, the relationship is complex and requires careful specialist evaluation. Cryptogenic stroke in children is itself extremely rare.
In Adults: A Different Conversation
Much of the literature and public information about PFO relates to adults, particularly in the context of migraine with aura and decompression illness in divers. These associations are largely irrelevant to children and should not cause unnecessary concern when a PFO is found in a young child or baby.
Dr. Giardini’s approach is to be clear with families about what the evidence actually shows in the paediatric context, rather than allowing adult-focused information to generate unnecessary anxiety.
Does a PFO Need Treatment?
Almost Never in Children
The vast majority of children with a PFO need no treatment at all: no medication, no surgical intervention, and no restrictions on physical activity or sport. The finding can, in most cases, simply be noted and the family reassured.
Closure: Only in Very Specific Circumstances
PFO closure is a catheter-based procedure in which a small device is used to seal the opening. It is occasionally considered in adults, principally following a cryptogenic stroke where all other causes have been excluded. In children, closure is extremely rarely indicated and would only be discussed in the context of a very specific clinical scenario, having weighed all the evidence carefully. It is not a routine procedure and should never be performed without a clear, compelling indication.
What Follow-up Is Needed?
In most cases, no follow-up at all is required. Once the finding has been properly assessed and the family reassured, there is no need for repeat echocardiograms or ongoing cardiology reviews.
Occasionally, a single follow-up appointment may be appropriate, for example if the PFO was found in the context of a broader cardiac assessment, or if the family would benefit from the opportunity to ask further questions once they have had time to digest the information.
When Should I See a Paediatric Cardiologist?
If your child has been told they have a PFO and you are uncertain what it means, a single consultation with a paediatric cardiologist can be enormously reassuring. Most of these consultations end with a clear, confident explanation and discharge: no further investigations, no treatment plan, simply the peace of mind that comes from expert assessment.
More specifically, a specialist opinion is worth seeking if your child has unexplained neurological symptoms, a history of stroke or TIA, or a complex medical background where the significance of the PFO is genuinely uncertain.
Frequently Asked Questions
Is a PFO the Same as a Hole in the Heart?
Not exactly. The term “hole in the heart” is most often used to describe atrial septal defects (ASDs), which are true structural defects requiring monitoring and sometimes treatment. A PFO is different. It is a remnant of a normal fetal structure that has simply not sealed completely, rather than an abnormal opening. The distinction matters: most ASDs require follow-up, while most PFOs do not.
My Child Was Born with a PFO. Will It Close on Its Own?
Many PFOs do close spontaneously in the first months of life. In those that remain open, the opening itself tends to be small and functionally insignificant. A PFO that persists into childhood or adulthood usually remains clinically unimportant throughout life.
Can My Child Play Sport with a PFO?
Yes. There are no activity restrictions for children with an isolated PFO. The heart functions normally and there is no increased cardiac risk during exercise. Children with a PFO can participate fully in all sports and physical activities.
Will My Child Need Surgery?
Almost certainly not. PFO closure in children is extremely rarely indicated and is reserved for a very small number of highly specific situations. For the vast majority of children, no intervention of any kind is needed.
Could the PFO Have Caused My Child’s Symptoms?
If your child has chest pain, palpitations, fatigue, or breathlessness, these are very unlikely to be caused by a PFO. These symptoms deserve proper assessment, but the PFO itself should not be assumed to be the explanation. In clinic, Dr. Giardini takes time to ensure that any symptoms are properly understood and attributed, and not incorrectly blamed on an incidental finding.
Should I Be Worried?
No. A PFO in a child is, in the great majority of cases, an entirely benign finding with no implications for health, longevity, or quality of life. It is one of the commonest cardiac findings in the general population and is present in millions of healthy people worldwide.
Dr. Alessandro Giardini, MD, PhD
Written 05/04/2026

