What is Long QT Syndrome?
Long QT syndrome (often shortened to LQTS) is a condition that affects the electrical system of the heart. In simple terms, it means the heart takes a little longer than normal to reset between beats.
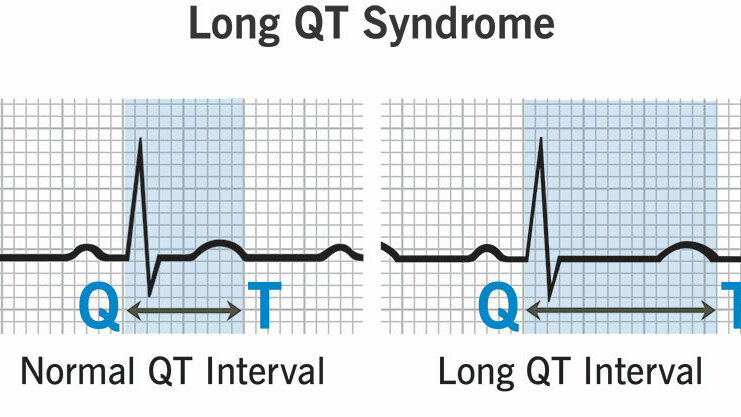
We see this on an ECG (electrocardiogram) as a prolonged “QT interval”. When that interval is too long, the heart becomes more vulnerable to slipping into a dangerous rhythm, called torsades de pointes.
If that happens, a child may suddenly faint. Very rarely, it can lead to cardiac arrest. This is why, although many children are completely well, the condition deserves proper attention.
Long QT syndrome is not particularly rare. It affects around 1 in 2,000 people and is an important cause of unexplained faints or sudden events in otherwise healthy children and teenagers.
What causes it?
In most cases, Long QT syndrome is inherited. It is caused by a change in one of the genes that control how electrical signals move through the heart.
There are a few main types, and each behaves slightly differently. Some children are more likely to have symptoms during exercise, particularly swimming. Others may be triggered by sudden noises, like an alarm going off at night. In a smaller group, events tend to happen at rest or during sleep.
Because it is inherited, there is often a family pattern, although not always an obvious one. A parent may carry the gene without ever having had symptoms.
Less commonly, the QT interval can become prolonged because of external factors. Certain medications, electrolyte imbalances (like low potassium), or acute illness can all temporarily affect the heart’s electrical system. In these cases, the problem is often reversible once the underlying cause is addressed. A very useful resource for checking medications is CredibleMeds.org.
What symptoms should parents look out for?
One of the tricky things about Long QT syndrome is that many children have no symptoms at all. Quite often, the diagnosis comes to light only after another family member is identified.
When symptoms do occur, they are usually quite striking. The most common one is a sudden faint. This can happen during exercise, when a child is upset, or sometimes just after being startled. It often comes without much warning, which is one of the clues that this is not a simple faint.
Some children are initially thought to have epilepsy, because a prolonged faint can be accompanied by brief jerking movements. Others describe episodes of their heart racing or fluttering.
Thankfully, cardiac arrest as a first presentation is rare, but Long QT syndrome is one of the conditions we always think about when a young person collapses unexpectedly.
If there is any doubt, this is exactly the sort of situation where I would strongly recommend a proper assessment by a paediatric cardiologist.
How is Long QT syndrome diagnosed?
The starting point is always an ECG. This allows us to measure the QT interval and correct it for heart rate (QTc). In children, a QTc of around 460 milliseconds or more would raise concern, and values above 500 milliseconds are associated with a higher risk.
That said, it is not always straightforward. Some children with genuine Long QT syndrome can have a normal ECG at rest. For that reason, we often go a step further.
An exercise test can be very helpful, as it shows how the QT interval behaves when the heart rate increases and then recovers. In some cases, genetic testing is also arranged. This can confirm the diagnosis and, importantly, allows us to screen other family members.
Family screening is absolutely key. In many cases, we identify relatives who were completely unaware they carried the condition.
How is it treated?
The reassuring part is that, once diagnosed, Long QT syndrome is usually very manageable.
Most children are treated with a beta-blocker, such as propranolol or nadolol. These medications reduce the effect of adrenaline on the heart and significantly lower the risk of dangerous rhythms. They are generally very well tolerated and form the backbone of treatment.
Alongside medication, we talk through practical day-to-day considerations. This might include being sensible around certain triggers, checking medications carefully, and making sure schools are aware of the diagnosis. Children can and should remain active, but occasionally we tailor advice depending on the specific type of LQTS.
In a small number of higher-risk cases,, particularly if a child has already had a serious event or continues to have symptoms despite medication—we may recommend an implantable defibrillator (ICD). This is a device that can automatically correct a dangerous rhythm if it occurs.
There is also a surgical option called left cardiac sympathetic denervation, which is used in selected situations.
What does this mean for my child’s future?
This is usually the first question parents ask, and understandably so.
The honest answer is that, with the right treatment and a bit of awareness, the vast majority of children with Long QT syndrome grow up to live completely full and active lives. They go to school, play sports, and do all the normal things you would expect.
The key is recognising the condition early and putting the right measures in place.
Common questions I get asked in clinic
Parents often ask whether their child has to stop sport altogether. In most cases, the answer is no. We might adapt things slightly depending on the situation, but we very rarely advise children to avoid activity completely.
Another common question is whether parents or siblings should be tested. The answer here is yes because this is an inherited condition, checking close family members is an essential part of care.
I am also often asked whether a normal ECG rules things out. Unfortunately, it does not entirely. If the story suggests Long QT syndrome, we still need to look a bit deeper.
Some parents wonder whether this is the same as Brugada syndrome. It is not. They are different conditions, although both affect the heart’s electrical system.
What should I do if my child collapses?
If your child loses consciousness suddenly and unexpectedly, you should call 999 immediately.
If they are not breathing normally, start CPR straight away. It is well worth learning basic life support as a family. Organisations such as the British Heart Foundation and St John Ambulance offer excellent courses.
In some families, we also discuss whether having a home defibrillator is appropriate.
When should you see a specialist?
If your child has had an unexplained faint, has been diagnosed with epilepsy without a clear cause, or there is a family history of sudden death, it is important to have a proper cardiac assessment.
This is very much an area where seeing an experienced paediatric cardiologist makes a real difference. If you are unsure, I am always happy to review symptoms and advise on whether further testing is needed.
Dr. Alessandro Giardini, MD, PhD
Consultant Paediatric Cardiologist, Great Ormond Street Hospital and The Portland Hospital
Written 26/03/2026