Kawasaki Disease in Children: A Parent’s Guide to Diagnosis, Treatment and Recovery
Written by Dr Alessandro Giardini, Consultant Paediatric Cardiologist, London
If your child has been diagnosed with Kawasaki disease — or you suspect they might have it — it is completely understandable to feel worried. Kawasaki disease is one of the most common causes of acquired heart disease in children in the United Kingdom, yet many parents have never heard of it until their own child falls ill. This guide explains what Kawasaki disease is, how it is diagnosed and treated in the UK, what the latest research tells us, and what you can expect during your child’s recovery.
What Is Kawasaki Disease?
Kawasaki disease is an acute illness that causes inflammation of the blood vessels (vasculitis) throughout the body. It predominantly affects children under the age of five, although older children and, very rarely, adults can develop it too. In the UK, approximately 8 in every 100,000 children under five are affected each year, making it uncommon but far from rare.
The condition was first described by Dr Tomisaku Kawasaki in Japan in 1967. It is more common in children of East Asian descent, but it occurs in children of all ethnic backgrounds. Boys are affected roughly 1.5 times more often than girls.
The most important concern with Kawasaki disease is the effect it can have on the coronary arteries — the blood vessels that supply the heart muscle. Without timely treatment, approximately 20 to 25 per cent of children can develop coronary artery abnormalities, including potentially serious coronary artery aneurysms. With prompt diagnosis and treatment, however, this risk drops to below 5 per cent.
What Causes Kawasaki Disease?
The exact cause of Kawasaki disease remains unknown. Current research suggests it is triggered by an abnormal immune response most likely to an infection and in children who are genetically predisposed. It is not contagious and cannot be passed from one child to another. You cannot catch it from another family, and it is not caused by anything a parent has done or not done.
During the COVID-19 pandemic, researchers observed an increase in Kawasaki-like symptoms in some children. A condition called Paediatric Inflammatory Multisystem Syndrome Temporally associated with SARS-CoV-2 (PIMS-TS), also known as Multisystem Inflammatory Syndrome in Children (MIS-C), shares features with Kawasaki disease but is now recognised as a distinct condition. Your doctor will be able to distinguish between the two.
Symptoms of Kawasaki Disease: What to Look For
Kawasaki disease presents with a characteristic combination of symptoms. As a parent, knowing these signs can help you seek medical attention promptly, which is critical for effective treatment.
The Key Features
A diagnosis of complete (typical) Kawasaki disease is made when a child has a fever lasting five days or more together with at least four of the following five clinical features:
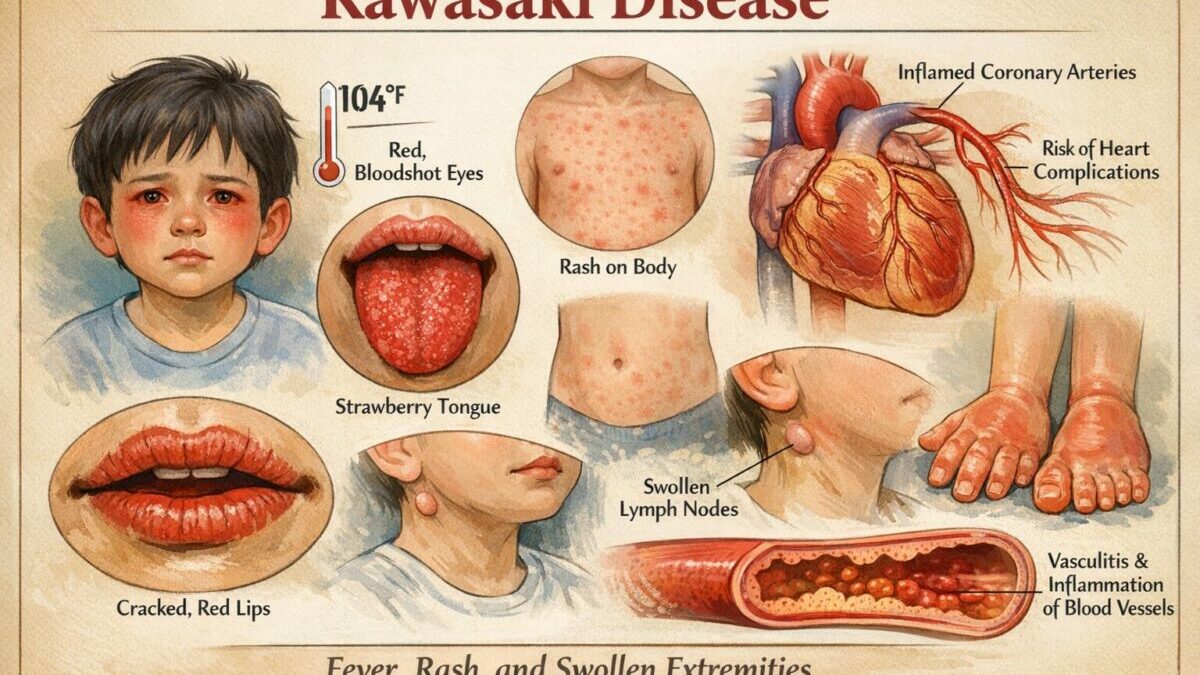
1. Changes to the eyes: Both eyes become red and bloodshot (bilateral conjunctival injection) without any sticky discharge or pus. This is different from conjunctivitis.
2. Changes to the lips and mouth: The lips may become dry, cracked, and bright red. The tongue can swell and develop a bumpy, red appearance often described as a “strawberry tongue.” The lining of the mouth and throat may also be red.
3. Skin rash: A widespread rash can appear on the body, often on the trunk and groin area. The rash can take many forms and may look different from child to child.
4. Changes to the hands and feet: The fingers and toes may become swollen, red, and puffy. Later in the illness (usually after 10 to 14 days), the skin on the fingertips and toes often begins to peel.
5. Swollen lymph node in the neck: A single enlarged, firm lymph node (at least 1.5 cm) is often found on one side of the neck.
Incomplete (Atypical) Kawasaki Disease
Some children, particularly those under one year of age, may not develop all five features. This is called incomplete or atypical Kawasaki disease, and it can be harder to diagnose. It is especially important to be aware of this because younger children are at a higher risk of developing coronary artery complications. The updated 2024 American Heart Association scientific statement emphasises that clinicians should maintain a high index of suspicion in any child with prolonged unexplained fever, even when fewer than four of the classic features are present.
Other Symptoms Parents May Notice
In addition to the classic features, children with Kawasaki disease may also experience irritability (often marked and unexplained), joint pain and swelling, abdominal pain, diarrhoea or vomiting, and a small, fluid-filled swelling at the site of a previous BCG vaccination. Extreme irritability in a young child with fever should always prompt medical attention.
How Is Kawasaki Disease Diagnosed?
There is no single blood test that can confirm Kawasaki disease. The diagnosis is made clinically, meaning it is based on the pattern of symptoms your child presents with, combined with supportive blood test results and exclusion of other conditions.
Blood Tests and Investigations
Your child’s medical team will typically carry out several investigations, including blood tests looking for markers of inflammation such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR), a full blood count (which may show raised white blood cells and platelets), liver function tests, and a urine test.
Crucially, an echocardiogram (heart ultrasound) will be performed to assess the coronary arteries and heart function. This is a painless, non-invasive scan. Even if the initial echocardiogram is normal, repeat scans are an essential part of follow-up care.
The 2024 AHA scientific statement highlights the role of emerging diagnostic tools, including machine learning algorithms that use routine blood tests to help distinguish Kawasaki disease from other febrile illnesses in the early stages, though these are not yet in routine clinical practice in the UK.
Treatment of Kawasaki Disease: The UK Approach
Prompt treatment is essential. The goal is to reduce inflammation quickly and prevent damage to the coronary arteries. In the UK, treatment follows established protocols aligned with national and international guidelines.
First-Line Treatment: IVIG and Aspirin
The standard first-line treatment is intravenous immunoglobulin (IVIG): a high-dose infusion of antibodies given directly into a vein over several hours. This is usually given as a single dose of 2 g/kg body weight. Treatment is most effective when given within the first 10 days of illness, ideally as early as possible once the diagnosis is made.
Alongside IVIG, your child will be started on aspirin. Initially this is given at a high dose to help reduce inflammation and fever. Once the fever resolves and inflammation markers improve, the dose is reduced to a lower level (typically 3–5 mg/kg/day) which helps prevent blood clots. Low-dose aspirin is usually continued for six to eight weeks, or longer if there are coronary artery changes.
Identifying High-Risk Children
The 2024 AHA update introduced a refined approach to identifying children at higher risk of developing coronary artery aneurysms. Risk factors include age under 6 months, Asian ethnicity, elevated coronary artery z-scores at baseline, and very high inflammatory markers (CRP of 13 mg/dL or above). Children identified as high-risk may be considered for more intensive initial treatment.
Adjunctive and Second-Line Treatments
Some children may be treated with corticosteroids (such as prednisolone or methylprednisolone) alongside IVIG, particularly if they are identified as being at high risk. Recent evidence, including the updated 2024 AHA statement, supports the use of corticosteroids as adjunctive therapy in selected patients to further reduce the risk of coronary artery complications.
Approximately 10 to 20 per cent of children do not respond to the first dose of IVIG: their fever returns or persists. These children are described as having IVIG-resistant Kawasaki disease. Treatment options for resistant cases include a second dose of IVIG, intravenous methylprednisolone, or infliximab (a biologic anti-inflammatory medication). More recently, other agents such as anakinra (an interleukin-1 receptor antagonist) have been studied, and the 2024 AHA statement discusses their emerging role.
Treatment for Coronary Artery Aneurysms
If your child develops coronary artery aneurysms, additional medications may be required to prevent blood clots from forming inside the aneurysm. These can include continued low-dose aspirin, clopidogrel (another antiplatelet medication), and in more severe cases, anticoagulants such as warfarin. The 2024 AHA statement notes emerging data supporting the use of direct oral anticoagulants in selected patients, though this remains an area of active research.
Follow-Up Care After Kawasaki Disease
Even after your child has recovered from the acute illness, follow-up is essential. In the UK, follow-up typically involves the following schedule.
A repeat echocardiogram is usually performed at two weeks and again at six to eight weeks after the onset of illness. If the coronary arteries are normal on all scans and the child has recovered well, low-dose aspirin is usually stopped at around six to eight weeks and no further cardiac follow-up may be needed.
Children who develop coronary artery changes will need long-term follow-up with a paediatric cardiologist. The frequency and nature of follow-up depends on the severity of the coronary artery involvement and may include regular echocardiograms, and in some cases, CT coronary angiography or cardiac MRI as the child grows older.
As a paediatric cardiologist in London, I see children at all stages of Kawasaki disease from initial diagnosis through to long-term follow-up. If your child has been diagnosed with Kawasaki disease and you would like a specialist cardiac assessment or a second opinion, I am happy to help.
What the Latest Research Tells Us (2024–2025)
Kawasaki disease research continues to advance rapidly. Some of the most important recent developments include the following.
The 2024 American Heart Association (AHA) Scientific Statement, the most comprehensive update since 2017, has refined the approach to identifying high-risk patients and expanded the discussion of treatment options beyond IVIG, including updated guidance on corticosteroids, infliximab, anakinra. It also includes new recommendations for long-term imaging surveillance and anticoagulation in patients with coronary artery aneurysms.
New imaging techniques, including advanced echocardiographic methods and cardiac MRI, are improving our ability to detect subtle coronary artery changes and monitor long-term heart health in children who have had Kawasaki disease.
Research into the genetic basis of Kawasaki disease and the development of more targeted therapies, including biologics and immunomodulators, continues, with the hope of offering more personalised treatment approaches in the future.
Kawasaki Disease and Your Child’s Heart: Why Specialist Cardiology Follow-Up Matters
The heart is the organ most at risk from Kawasaki disease. Inflammation of the coronary arteries can lead to aneurysms (weakened, ballooning segments of the artery), stenosis (narrowing), or, in rare untreated cases, thrombosis (blood clots). This is why every child with Kawasaki disease should have an echocardiogram and be assessed by a paediatric cardiologist.
The good news is that with early diagnosis and treatment, the vast majority of children make a full recovery with no lasting heart damage. For those who do develop coronary changes, modern treatments and careful long-term monitoring mean that outcomes are significantly better than they were even a decade ago.
Frequently Asked Questions About Kawasaki Disease
Below are some of the questions I get most commonly asked:.
1. What are the first signs of Kawasaki disease in a child?
The first and most important sign is a persistent high fever (usually above 38.5°C) that lasts for five days or more and does not respond well to paracetamol or ibuprofen. Over the following days, other features may develop: red eyes without discharge, a rash on the body, red or cracked lips, a “strawberry” tongue, swollen hands or feet, and a swollen gland on one side of the neck. Not all children develop every symptom, and symptoms may come and go.
2. Is Kawasaki disease serious?
Yes, Kawasaki disease should be taken seriously. Without treatment, it can cause damage to the coronary arteries (the blood vessels that supply the heart) in up to 25 per cent of children. However, when diagnosed and treated promptly with IVIG (ideally within the first 10 days of illness) the risk of serious heart complications drops to below 5 per cent. The vast majority of children treated early make a full and complete recovery.
3. What causes Kawasaki disease?
The precise cause is still unknown. It is thought to be an abnormal immune response, possibly triggered by an infection in genetically susceptible children. It is not caused by anything a parent has done, and it is not contagious. You cannot catch Kawasaki disease from another child, and siblings are very rarely affected.
4. Can Kawasaki disease damage the heart permanently?
In most children who receive timely treatment, there is no permanent heart damage. However, a small number of children may develop coronary artery aneurysms, which require long-term monitoring and, in some cases, ongoing medication. The severity of coronary artery involvement varies considerably. Children with small aneurysms often see them resolve over time, while larger aneurysms may persist and need lifelong follow-up with a paediatric cardiologist.
5. How is Kawasaki disease treated in the UK?
In the UK, the standard treatment is a high-dose infusion of intravenous immunoglobulin (IVIG) given as a single dose of 2 g/kg, alongside aspirin. High-risk children may also receive corticosteroids. If a child does not respond to the initial IVIG treatment, a second dose of IVIG, intravenous steroids, or infliximab may be considered. Treatment is delivered in hospital and children are usually monitored for at least 24 to 48 hours after IVIG.
6. Can Kawasaki disease come back?
Recurrence is uncommon but possible. If your child develops a prolonged fever with any of the characteristic features again, even months or years later, you should seek medical attention and mention the previous diagnosis.
7. When can my child go back to school or nursery?
Most children can return to school or nursery once they are feeling well, the fever has fully resolved, and they have enough energy to participate normally. This is typically within one to two weeks of leaving hospital. However, if your child is taking low-dose aspirin, it is worth informing the school and being aware of the small increased risk of Reye’s syndrome if your child develops chickenpox or influenza while on aspirin. Your medical team will advise on appropriate precautions, including flu vaccination.
8. Does my child need to see a child heart specialist (paediatric cardiologist)?
Yes. Every child diagnosed with Kawasaki disease should have at least one echocardiogram and be reviewed by a paediatric cardiologist, even if the initial heart scan appears normal. Coronary artery changes can sometimes develop after the acute illness has resolved, which is why follow-up echocardiograms at two weeks and six to eight weeks are standard. If any abnormalities are found, ongoing specialist follow-up will be arranged.
9. Is Kawasaki disease linked to COVID-19?
During the COVID-19 pandemic, a condition called PIMS-TS (Paediatric Inflammatory Multisystem Syndrome Temporally associated with SARS-CoV-2) was identified. PIMS-TS shares some features with Kawasaki disease, including fever, rash, and coronary artery involvement, but is now recognised as a distinct condition that occurs several weeks after SARS-CoV-2 infection. While the two conditions have similarities, they are managed slightly differently and have different age profiles. Your paediatrician or cardiologist will be able to differentiate between them.
10. Will my child be completely normal after Kawasaki disease?
For the majority of children, particularly those diagnosed and treated early, the answer is yes. Most children recover fully and go on to lead completely normal, healthy, and active lives with no restrictions. A small number of children with coronary artery involvement may need ongoing monitoring and, in some cases, medications for a period of time. Even in these cases, most children are able to participate in normal activities including sports, with guidance from their cardiologist. As a parent, the most important thing you can do is attend all follow-up appointments and raise any concerns with your child’s medical team.
Dr. Alessandro Giardini, MD, PhD
Written 30/03/2026