Hypertrophic Cardiomyopathy in Children: A Guide for Parents
By Dr Alessandro Giardini, Senior Consultant Paediatric and Adolescent Cardiologist, London, UK
Being told that your child has hypertrophic cardiomyopathy (HCM) is a lot to take in. The diagnosis sounds serious, and the questions that follow come fast: what will this mean for school, for sport, for the years ahead?
What most families find, once the initial shock settles, is that the picture is considerably more reassuring than they feared. With the right diagnosis and specialist input, most children with HCM do well and can remain active, although some adjustments are sometimes needed. Dr Giardini is experienced in managing children with HCM. This page aims to give you a clear, honest, and practical account of what the condition involves.
Key Facts About Hypertrophic Cardiomyopathy in Children
- HCM is a genetic condition that causes the heart muscle to become abnormally thickened
- Many children, particularly those found through family screening, have no symptoms at all
- It often runs in families, making screening of relatives an important part of management
- The risk of serious heart rhythm problems exists but is low for most children
- The majority of children are monitored carefully and do not require immediate treatment
What is Hypertrophic Cardiomyopathy?
Hypertrophic cardiomyopathy is a condition in which the heart muscle, most often the wall of the left ventricle, which is the heart’s main pumping chamber, becomes abnormally thick. This thickening creates two main problems. The muscle can become stiff, making it harder for the heart to relax and fill between beats. And in a significant proportion of children, roughly one in three at rest, and more during exertion, the thickened muscle can partially block the flow of blood out of the heart, a pattern known as obstructive HCM or HOCM.
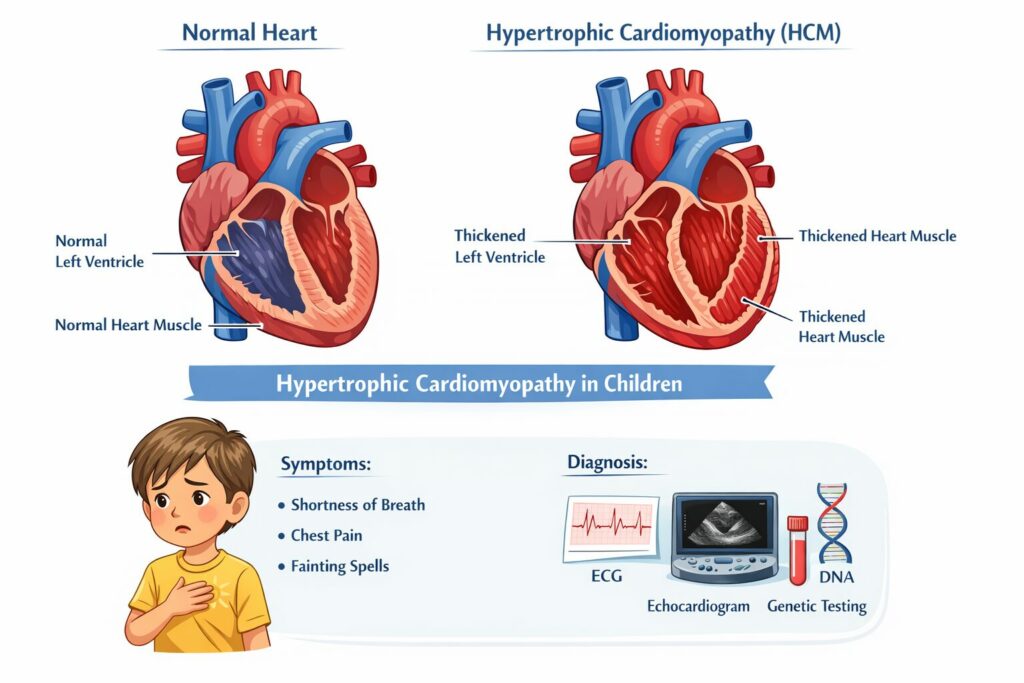
HCM is not a single, uniform condition. It encompasses a range of related disorders, and the outlook depends significantly on the underlying cause, the extent of thickening, and the age at which the diagnosis is made. Children diagnosed in infancy require particularly careful evaluation, as the range of possible causes at that age is considerably broader than in older children and teenagers.
What Causes Hypertrophic Cardiomyopathy in Children?
In older children and teenagers, HCM is most commonly the result of an inherited genetic change, specifically a pathogenic variant in one of the genes responsible for the structure of the heart muscle sarcomere, the fundamental unit of cardiac contraction. The genes most frequently involved are MYH7 and MYBPC3.
This form of HCM follows an autosomal dominant inheritance pattern: there is a one in two chance that it has been passed on from a parent, which is why family screening is such an important part of the assessment.
In younger children and infants, the picture is more varied. Up to a third of cases in this age group arise from conditions other than sarcomere gene variants, including metabolic storage diseases (such as Pompe disease or Danon disease), RASopathies (such as Noonan syndrome), mitochondrial disorders, and neuromuscular conditions. Establishing the precise underlying cause in these children is not merely academic as several of these conditions now have targeted treatments available, making an accurate diagnosis directly relevant to management.
In some children, no identifiable cause is found, and the HCM is classified as idiopathic. Careful monitoring and family screening remain important regardless.
What Are the Symptoms of HCM in Children?
A substantial number of children with hypertrophic cardiomyopathy, particularly those identified through family screening before any problems arise, experience no symptoms whatsoever.
When symptoms do occur, they most commonly include breathlessness or reduced stamina during exercise, chest pain or tightness, palpitations, and lightheadedness or fainting, particularly in relation to physical activity.
Fainting during or immediately after exercise requires prompt specialist evaluation and should never be attributed to a simple faint or dehydration without thorough cardiac assessment.
HCM is also one of the recognised causes of sudden cardiac arrest in young people during sport, though the absolute risk for any individual child is low. A central part of specialist HCM management is identifying the minority of children who are at higher risk, so that appropriate steps can be taken.
How is Hypertrophic Cardiomyopathy Diagnosed?
Assessment begins with a detailed clinical history, including a careful review of any symptoms and a thorough family history. A resting ECG is always performed and is frequently abnormal in HCM even when no symptoms are present. This sometimes providing the first indication that further investigation is warranted.
The cornerstone of diagnosis is the echocardiogram, which allows direct measurement of the heart wall thickness and assessment of how the heart fills, contracts, and whether any obstruction to outflow is present. In children, all measurements must be interpreted in relation to body size rather than against adult reference values.
Depending on the clinical picture, further investigations may include cardiac MRI which provides detailed structural information and can identify areas of fibrosis, ambulatory ECG monitoring to detect rhythm disturbances, and exercise stress testing to evaluate how the heart and blood pressure respond to exertion.
Genetic testing is recommended in most children. It supports an accurate diagnosis and is the most efficient basis for screening other family members. In younger children, additional metabolic and genetic investigations may be needed to identify or exclude treatable underlying causes.
What Treatments Are Available?
Management is tailored to each child individually. Many children require monitoring rather than immediate medication, and the overall aim is to manage symptoms, reduce risk, and preserve as good a quality of life as possible.
Medication. Beta-blockers are generally first-line treatment, reducing heart rate and allowing the ventricle more time to fill. Calcium channel blockers such as verapamil are used where beta-blockers are not tolerated. Mavacamten, a newer cardiac myosin inhibitor licensed in adults with obstructive HCM, is currently under evaluation in adolescents and may become a relevant option in younger patients in the coming years.
Septal reduction therapy. Where obstruction remains severe despite medication and is associated with symptoms, surgical myectomy (the careful removal of a small portion of the thickened muscle) is the most established and effective procedure. This procedure results in excellent outcomes at specialist centres.
ICD implantation. Children at higher risk of life-threatening ventricular arrhythmia may be recommended an implantable cardioverter-defibrillator. This decision is guided by validated paediatric risk assessment tools (including the ESC HCM Risk-Kids approach) alongside a detailed individual clinical evaluation and open discussion with the family.
Exercise and sport. This is among the most frequently raised concerns at clinic, and rightly so. The majority of children with HCM should remain physically active and moderate exercise is actively encouraged. High-intensity competitive sport carries a potentially higher risk and requires individual assessment rather than blanket restriction. Dr Giardini provides tailored, evidence-based guidance aimed at keeping children as active as is safely appropriate for their specific situation.
Monitoring. HCM can evolve with growth, particularly during the adolescent years. Regular review with echocardiogram, ECG, and ambulatory monitoring adjusted to each child’s findings and risk profile is an essential part of long-term management.
Frequently Asked Questions
Can hypertrophic cardiomyopathy be cured in children?
There is currently no cure for inherited HCM. However, with appropriate monitoring and management, most children have a good long-term outlook. Where HCM arises from a specific metabolic cause, targeted treatments are increasingly available.
Does a child with HCM always need medication?
Not always. Many children without symptoms are managed initially through careful monitoring rather than medication, with treatment introduced if and when the clinical picture warrants it.
Should other family members be tested?
Yes. Parents and siblings should undergo clinical cardiac screening, and genetic testing is recommended where a pathogenic variant has been identified, allowing relatives to be assessed efficiently.
Can a child with HCM play sport?
In most cases, yes with appropriate guidance. Moderate physical activity is encouraged for the majority of children. Competitive high-intensity sport requires individual assessment taking into account the degree of thickening, any obstruction, and the results of further investigation.
What is the risk of sudden cardiac death in children with HCM?
The overall risk is low but not zero. The majority of children with HCM are assessed as low risk. A smaller number have features that place them in a higher-risk category, where protective measures such as ICD implantation may be considered.
Does HCM worsen over time?
In some children the condition remains stable over many years. In others, particularly during the growth of adolescence the degree of muscle thickening can increase. This is one of the reasons why regular specialist review throughout childhood is so important.
Will my child need lifelong follow-up?
Yes. HCM is a condition that requires lifelong cardiac care. Planning the transition from paediatric to adult cardiology services is something Dr Giardini addresses with families well in advance, to ensure continuity of specialist care as the child moves into adulthood.
Where Can I See a Paediatric Cardiologist in London?
Dr Alessandro Giardini sees children with hypertrophic cardiomyopathy across several locations in London, UK. Dr. Giardini works with and has direct access to leading specialists in all disciplines related to HCM including clinical genetic, cardiac imaging, electrophysiology and cardiac surgery. Families are welcome to self-refer, or to be referred by their GP or paediatrician.
Dr. Alessandro Giardini, MD, PhD
Written 01/04/2026