This page explains what AVSD is, what causes it, what symptoms to look for, how it is treated, and what you can expect for your child’s future. It has been written by Dr. Alessandro Giardini to give families the kind of clear, practical information that is often hard to find in the immediate aftermath of a diagnosis.
What Is an Atrioventricular Septal Defect?
An atrioventricular septal defect is a congenital heart condition, meaning it is present from birth, that affects the centre of the heart. To understand it, it helps to know a little about how the normal heart is structured.
In a healthy heart, the two upper chambers (the atria) are separated from each other by a wall called the atrial septum, and the two lower chambers (the ventricles) are separated by the ventricular septum. There are two separate valves controlling blood flow between the upper and lower chambers on each side: the mitral valve on the left and the tricuspid valve on the right.
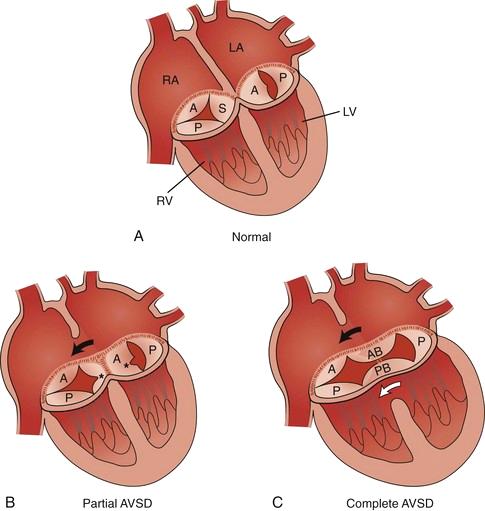
In a heart with AVSD, the development of the central part of the heart is incomplete. There is a gap between the atria, a gap between the ventricles, and instead of two separate valves, there is a single shared valve sitting across the middle. This means that blood flows abnormally through the heart, mixing between the left and right sides, and more blood than normal is directed to the lungs. Over time, this places strain on the heart and lungs, which is why surgical repair is needed. There are 2 main types of AVSD as we will see later on: the partial (B) and the complete form (C).
AVSD accounts for around four to five per cent of all congenital heart defects. It is one of the conditions that paediatric cardiologists and cardiac surgeons see regularly, and one for which outcomes have improved substantially over recent decades.
What Causes AVSD?
AVSD develops early in pregnancy, during the fifth to eighth weeks of gestation, when the central structures of the heart are forming. An area of tissue called the endocardial cushions, which is responsible for forming the lower part of the atrial septum, the upper part of the ventricular septum, and the atrioventricular valves, fails to develop fully. The result is the characteristic combination of defects seen in AVSD.
It is important for parents to understand that this is not caused by anything they did or did not do during pregnancy. In the majority of cases, no single clear cause is identified. AVSD is, however, more common in children with Down syndrome (trisomy 21), with approximately half of all complete AVSDs occurring in children with this chromosomal condition. AVSD can equally occur in children with no associated genetic condition, and the presence of Down syndrome does not change the fundamental surgical approach or the excellent outlook after repair.
Types of AVSD
Understanding which type of AVSD your child has is important, because it influences the timing and nature of treatment.
Complete AVSD
Complete AVSD is the more significant form, involving a large central defect with gaps between both the atria and the ventricles, and a single common valve. Because blood flows freely between all four chambers of the heart, symptoms tend to appear early in life and can be significant. Surgery is typically planned within the first three to six months of life.
Partial AVSD
In partial AVSD, the defect is less extensive. There is usually a gap between the upper chambers (an ostium primum atrial septal defect), but the ventricular septum is intact. The mitral valve on the left side is often abnormal, with a gap in one of its leaflets called a cleft. Children with partial AVSD may have few or no symptoms initially, and in some cases the diagnosis is not made until a heart murmur is detected during a routine check. Because symptoms are milder, surgery can often be planned for later in childhood, typically between the ages of three and eight years.
Transitional AVSD
A transitional form sits between the two, sharing features of both. The distinction between subtypes is assessed carefully during echocardiographic evaluation and guides the specialist team’s planning.
What Are the Symptoms of AVSD?
Symptoms depend on the type and size of the defect and the degree to which the valve is leaking.
Symptoms in Complete AVSD
In complete AVSD, symptoms usually appear in the first weeks of life and may include fast or laboured breathing, difficulty feeding and tiring quickly during feeds, poor weight gain despite adequate nutrition, sweating during feeds (a sign the heart is working hard), and a tendency to develop frequent chest infections. These symptoms reflect the extra work being placed on the heart and lungs by the abnormal blood flow.
Symptoms in Partial AVSD
Many children with partial AVSD have no symptoms at all in early childhood, or only mild breathlessness with exertion that may go unnoticed. The condition is often picked up when a doctor hears a heart murmur during a routine examination. In some children, if the condition is not detected early, symptoms such as easy fatigue or reduced exercise tolerance may develop over time as the heart adapts to the abnormal circulation.
How Is AVSD Diagnosed?
The cornerstone of diagnosis is the echocardiogram, an ultrasound scan of the heart that shows both its structure and the pattern of blood flow through it in real time. The echocardiogram can define the type and extent of the defect, assess the valve anatomy and function, and provide the information needed to plan surgery.
AVSD may be diagnosed before birth, during routine pregnancy scanning, particularly the detailed anomaly scan at around 20 weeks of gestation. Antenatal diagnosis allows time for families to receive specialist counselling and for the birth to be planned at a centre with the right expertise. Alternatively, diagnosis may occur in the newborn period when symptoms prompt investigation, or later in childhood when a murmur leads to referral and echocardiography.
Additional investigations such as a chest X-ray and electrocardiogram (ECG) are often performed alongside the echocardiogram to provide further information about heart size, lung blood flow, and cardiac rhythm.
Treatment of AVSD
Surgery Is the Main Treatment
Surgery is the definitive treatment for AVSD. Unlike some simpler defects, AVSD does not close on its own, and the abnormal blood flow and valve function will cause progressive problems if not corrected. The operation is performed under general anaesthesia using cardiopulmonary bypass, which temporarily takes over the work of the heart and lungs while the surgeon operates.
The repair involves closing the holes in the heart using one or two patches of fabric material, dividing the single common valve into two separate valves, and repairing the valve leaflets to ensure they close properly and do not leak. The goal is to restore as normal a heart structure as possible in a single operation.
When Is Surgery Planned?
For complete AVSD, surgery is typically performed between three and six months of age, before the lungs are damaged by the prolonged exposure to high-pressure blood flow. Waiting too long risks the development of irreversible changes in the lung blood vessels (pulmonary vascular disease), which is why timely repair is important.
For partial AVSD, because symptoms are milder and the lungs are less affected, surgery is generally planned for beyond the first year of age, often around 2 years, when the risks of the operation are lower and the valve anatomy can be assessed more accurately.
Timing in each individual child is decided by the specialist team, taking into account the severity of symptoms, the degree of valve leakage, and the overall condition of the child.
What Happens During Recovery?
Following surgery, children spend time in a cardiac intensive care unit before moving to a general cardiac ward. The length of hospital stay varies depending on the complexity of the repair and how the child recovers, but most children are home within two to three weeks. Recovery at home is gradual, and families are given detailed guidance on wound care, activity, and follow-up before discharge.
What Are the Outcomes After Surgery?
The outcomes after AVSD repair are very good, and have continued to improve as surgical techniques and perioperative care have advanced. Most children who undergo repair go on to grow and develop normally, with good heart function and no significant activity restrictions.
Survival rates are high. Contemporary data from major specialist centres show long-term survival rates of around 90 per cent at 10 and 15 years after repair, and newer surgical techniques are producing even better early results.
It is important for parents to understand that, while repair restores near-normal heart function in most children, ongoing follow-up is needed throughout life. The most common issue requiring attention over time is the function of the repaired left-sided valve, which can develop a degree of leakage (regurgitation) as the child grows. A minority of children, estimated at roughly 10 to 15 per cent over 10 to 15 years, will require a further procedure related to valve function at some point in their lives. This is not a failure of the initial surgery; it reflects the nature of the condition and the way in which valves change as the heart matures. Regular follow-up ensures that any such changes are detected early and managed at the right time.
Long-Term Care and Follow-up
Children with AVSD are followed by a paediatric cardiologist throughout childhood and into adult life. The frequency of review is tailored to each child, but typically involves echocardiographic assessment at regular intervals to monitor valve function, heart size, and overall cardiac performance.
As children grow older and their hearts mature, follow-up often becomes less frequent if the repair is functioning well. Many young adults who had AVSD repair in infancy lead completely normal lives, with no restrictions on work, exercise, or starting a family, though they remain under the care of an adult congenital heart disease service.
Dr. Giardini’s work in congenital heart disease at Great Ormond Street Hospital encompasses both the initial assessment and surgical planning phase and the long-term follow-up of children with complex cardiac conditions, including AVSD. The goal of long-term care is to ensure each child reaches adulthood with the best possible heart function and quality of life.
Can My Child Live a Normal Life?
For the vast majority of children, the answer is yes. After successful repair, most children attend school normally, participate fully in sports and physical activities, and have no significant restrictions on daily life. Each child is assessed individually, and specific advice about activity is given based on the findings at follow-up, but the expectation for most families is one of genuine normality.
When Should You Seek Specialist Advice?
If your child has been diagnosed with AVSD, they will usually already be under specialist cardiac care. However, a specialist consultation is particularly valuable if you would like a second opinion on the diagnosis or the proposed surgical plan, if you want a clearer explanation of what the surgery involves and what to expect, or if you are uncertain about timing, long-term outlook, or the significance of valve findings on a recent echo.
Frequently Asked Questions
Is AVSD the Same as a Hole in the Heart?
Not exactly. The term “hole in the heart” is most often used to describe simpler defects such as atrial septal defects (ASDs) or ventricular septal defects (VSDs), which involve only the walls between the chambers. AVSD includes holes in the heart but also involves the valves at the centre of the heart, making it a more complex condition. It is treated differently and requires more specialised surgical expertise.
Is the Surgery Safe?
AVSD repair is a well-established procedure performed routinely in specialist congenital heart centres, with outcomes that have improved considerably over the past two decades. As with all open heart surgery in infants and children, it carries risks, and families are counselled about these in detail by their surgical team. Overall, the great majority of children come through the surgery well and recover without serious complications.
Will My Child Need More Than One Operation?
Most children undergo a single definitive repair. However, because the repaired valve may develop changes over time as the child grows, a proportion of patients, around 10 to 15 per cent over the first 10 to 15 years, will need a further valve-related procedure at some point. This is monitored carefully at follow-up so that any intervention, if needed, is planned at the optimal time.
Is AVSD Genetic?
AVSD has a strong association with Down syndrome (trisomy 21), and around half of children with complete AVSD have this chromosomal condition. Genetic causes beyond trisomy 21 are less common but are sometimes identified. In many children, no genetic cause is found. Genetic counselling may be offered as part of the overall assessment, particularly if there is a family history of congenital heart disease.
Does Down Syndrome Affect the Surgical Outcome?
The presence of Down syndrome does not change the fundamental surgical approach to AVSD, and outcomes after repair are comparable in children with and without Down syndrome. Children with Down syndrome who have AVSD repaired in a timely fashion generally do well, and the surgery significantly improves their health and quality of life.
What Is the Long-Term Outlook?
Very good. The majority of children who have AVSD repaired in infancy or early childhood grow up to lead full, active lives with good heart function. Long-term follow-up is important to monitor valve function and ensure any issues are detected and managed early, but for most families the expectation is one of excellent health and genuine normality.
My Child Was Diagnosed Before Birth. What Happens Next?
An antenatal diagnosis of AVSD allows the team to plan carefully for birth and for the early weeks of life. Families are usually referred to a specialist paediatric cardiology centre before the baby is born, where they can meet the cardiologists and surgeons, understand the planned treatment, and ask questions in a supported environment. This preparation makes a significant difference to how families experience the postnatal period and the lead-up to surgery.
If your child has been diagnosed with AVSD and you would like specialist advice or a second opinion, Dr. Alessandro Giardini offers consultations at several London Locations. Referrals from GPs and paediatricians are welcome, and self-referral is also possible. Contact: info@childheartspecialist.com
Dr. Alessandro Giardini, MD, PhD
Written 05/04/2026

