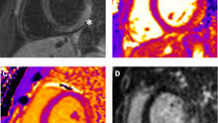
What is acute myocarditis in children?
Acute myocarditis is a sudden inflammation of the heart muscle (myocardium) in children and adolescents. When the heart muscle becomes inflamed, it can affect the heart’s ability to pump blood effectively throughout the body. Parents seeking information about myocarditis in children should understand that this is a rare but serious cardiac condition requiring specialist paediatric cardiology expertise.
Myocarditis affects approximately 1 per 100,000 children per year in the UK, though the true incidence is likely underestimated as mild cases may go unrecognised or be misdiagnosed. In children, myocarditis is most often acute (sudden onset) and can range from very mild symptoms to severe and life-threatening illness requiring intensive care support.
When infection or another trigger causes inflammation in the heart muscle, the body’s immune system responds by sending white blood cells to fight the infection. However, in myocarditis, this immune response can be overly aggressive, causing damage not just to the invading organism but also to the heart muscle cells themselves. Most damage is caused by the body’s immune reaction rather than by the infectious organism directly. The inflammation can affect a small area of heart muscle or involve a large portion, with more extensive damage generally causing more severe symptoms.
Myocarditis remains a recognised cause of sudden cardiac death in children and young athletes, which is why prompt diagnosis and specialist management by a paediatric cardiologist are essential. If you’re concerned your child may have symptoms of myocarditis in London or surrounding areas, you should seek urgent assessment from Dr Alessandro Giardini, Consultant Paediatric Cardiologist, who practices at Great Ormond Street Hospital and the Portland Hospital in London.
What causes acute myocarditis in children and adolescents?
Viral infections are by far the most common cause of myocarditis in children across the UK. Recent medical research has identified parvovirus B19 and human herpesvirus 6 as the most frequent viral causes of paediatric myocarditis, though coxsackievirus, adenovirus, Epstein-Barr virus, influenza, varicella (chickenpox), and common respiratory viruses can also be responsible. The virus enters the bloodstream and travels to the heart, where it infects heart muscle cells. As the virus replicates, the body’s immune system launches a response, releasing inflammatory substances such as tumor necrosis factor, interleukins, and nitric oxide that cause significant damage to the heart muscle.
COVID-19 has introduced new causes of myocarditis including direct infection with SARS-CoV-2 and multisystem inflammatory syndrome in children (MIS-C), which can develop weeks after COVID-19 infection involving the heart muscle and coronary arteries. Vaccine-associated myocarditis following mRNA COVID-19 vaccination has been reported, though children face much greater risk of myocarditis from COVID-19 infection itself than from vaccination.
Less commonly, bacterial and fungal infections can cause myocarditis, with newborns at particular risk as infections can pass from mother to baby during pregnancy or birth. Myocarditis can also occur as part of autoimmune diseases such as rheumatic fever, Kawasaki disease, or lupus, where the immune system mistakenly attacks the body’s own tissues. Rarely, certain medications, particularly chemotherapy drugs and some antibiotics, can trigger myocarditis through hypersensitivity reactions.
In many cases, despite thorough investigation, no specific cause is identified. These cases are labelled idiopathic myocarditis. It remains unclear why some children develop myocarditis when exposed to these triggers while most do not, though genetic factors or individual immune response variations may play a role. Males appear to have slightly higher risk than females. Because viral infections are the predominant cause and most damage occurs from the immune response rather than the virus itself, treatment focuses on supporting the heart while the inflammation resolves.
What are the symptoms of acute myocarditis in children?
The symptoms of acute myocarditis vary considerably, from very mild to severe, with younger children typically more severely affected due to immature immune systems. Newborns and infants may present with rapid or laboured breathing, poor feeding, extreme fussiness or unusual lethargy, pale or cool skin, reduced urine output, and fever. Neonatal myocarditis is often initially mistaken for sepsis, and symptoms can deteriorate rapidly.
Children over 2 years may be less severely symptomatic and commonly experience fatigue and weakness, chest pain or discomfort, abdominal pain and nausea from liver swelling, shortness of breath especially with activity, reduced exercise tolerance compared to peers, palpitations (awareness of rapid or irregular heartbeats), persistent cough, and dizziness. Fever can help distinguish myocarditis from other causes of heart dysfunction.
When myocarditis causes the heart to pump less effectively, children develop congestive heart failure with swelling in the face or legs, belly pain from liver swelling, reduced kidney function, rapid heartbeat at rest, and difficulty breathing when lying down. The challenge is that symptoms are often subtle early in the illness, making diagnosis difficult. Many children are initially thought to have respiratory illnesses like asthma or pneumonia, gastroenteritis, or simple flu. Some experience flu-like illness days or weeks before cardiac symptoms appear, while others seem completely well beforehand.
If your child in London or surrounding areas develops chest pain, severe breathing difficulty, significant fatigue disproportionate to activity, palpitations, or symptoms of heart failure, particularly following a recent viral illness, you should seek urgent specialist assessment. Given that myocarditis can deteriorate rapidly and symptoms may initially seem non-specific, evaluation by an experienced paediatric cardiologist is essential when there’s any concern about cardiac involvement.
How is acute myocarditis investigated by paediatric cardiologists?
Diagnosing acute myocarditis requires specialist paediatric cardiology expertise as there’s no single definitive test. Diagnosis is largely clinical, based on combining detailed history, physical examination, and multiple investigations. A paediatric cardiologist takes a comprehensive history including recent viral illnesses, symptom progression, exercise tolerance, and family history, whilst examining for signs of heart failure, abnormal heart sounds, rapid heart rate, and breathing difficulties.
An electrocardiogram (ECG) records the heart’s electrical activity and may show abnormal rhythms, changes suggesting inflammation or injury, or conduction abnormalities, though it can be normal in some cases. An echocardiogram (cardiac ultrasound) is essential for assessing how well the heart pumps, whether chambers are enlarged, if there’s fluid around the heart, and valve function. This helps distinguish myocarditis from other causes of heart dysfunction.
Blood tests for cardiac biomarkers are crucial. Troponin, released when heart muscle is damaged, is frequently markedly elevated in myocarditis. BNP or NT-proBNP hormones indicate heart strain and help assess severity. Inflammatory markers like CRP and ESR may be elevated. Testing attempts to identify the causative organism through viral PCR, bacterial cultures, and specific viral antibody testing for parvovirus B19 and human herpesvirus 6, though often no organism is identified.
A chest X-ray may show an enlarged heart, fluid in the lungs, or enlarged liver, all suggesting heart failure. Cardiac MRI is increasingly important as it can detect inflammation, tissue characteristics specific to myocarditis, myocardial swelling, and scarring. However, it requires children to lie still for extended periods, often necessitating sedation in younger children.
Endomyocardial biopsy, historically the gold standard, involves taking a heart muscle sample for microscopic examination but carries risks, particularly in small children. It’s now reserved for specific situations where diagnosis is uncertain and results would change management. A paediatric cardiologist synthesises all available information to make the diagnosis. A child with recent viral illness, fever, cardiac symptoms, reduced heart function on echocardiogram, and markedly elevated troponin and BNP would be diagnosed with myocarditis even if MRI or biopsy were negative or not performed.
If you have concerns about your child’s symptoms in London, particularly following a viral illness, you can arrange a consultation with Dr Alessandro Giardini, Consultant Paediatric Cardiologist practicing at Great Ormond Street Hospital and The Portland Hospital in London, for comprehensive cardiac assessment.
What are the available treatments for acute myocarditis?
Treatment for acute myocarditis focuses primarily on supporting the heart while inflammation resolves, as most children recover with appropriate medical management. A paediatric cardiologist directs the treatment plan, often collaborating with intensive care specialists. Several children require admission to a Hospital and some require admission to a paediatric or cardiovascular intensive care unit for close monitoring, as myocarditis can deteriorate rapidly. Continuous heart rhythm monitoring detects dangerous arrhythmias, whilst blood pressure, oxygen levels, and organ function are carefully tracked.
Strict bed rest is important during the acute phase, as evidence suggests strenuous activity may harm the inflamed heart. Physical activity is restricted for several weeks depending on severity, with gradual supervised increase as the heart recovers. Supportive cardiac medications help the heart function whilst healing. Diuretics remove excess fluid that accumulates, relieving breathlessness and abdominal discomfort. ACE inhibitors or ARBs reduce the heart’s workload, whilst beta-blockers slow the heart rate and reduce oxygen demands. In severe cases, intravenous inotropic medications like milrinone or dobutamine help the heart pump more strongly, and vasopressors support dangerously low blood pressure.
Dangerous heart rhythm abnormalities may require antiarrhythmic medications or other interventions. Antiviral medications are rarely used as most damage occurs early before diagnosis. When autoimmune causes are identified or in severe cases, immunosuppressive treatments including intravenous immunoglobulin or corticosteroids may be used, with decisions made case-by-case. Myocarditis secondary to conditions like Kawasaki disease or rheumatic fever follows treatment guidelines for those primary conditions.
In severe cases where the heart fails despite maximum medical therapy, mechanical support may be life-saving. ECMO is a mechanical system that replicates temporarily the work of he heart and the lungs when those organs are not working sufficiently. In exceptional cases where severe heart damage occurs and the heart fails to recover despite all treatments, heart transplantation may ultimately be necessary.
After the acute phase, continued specialist cardiac care is essential. Children require regular follow-up appointments with echocardiograms and ECGs, gradual reintroduction of physical activity under medical supervision, monitoring for chronic myocarditis or heart failure development, and long-term medications if heart function hasn’t fully recovered. Children without permanent damage typically need annual check-ups initially, whilst those with residual heart damage require more frequent monitoring and may need lifelong medications and specialist care.
With appropriate treatment, about two-thirds of children achieve complete recovery. Prognosis depends partly on age, with newborns having higher risk compared to older children. However, children surviving the acute phase have very good long-term survival chances. Some may develop chronic myocarditis or reduced heart function from scarring, requiring ongoing management by a paediatric cardiologist.
Frequently Asked Questions About Myocarditis in Children
How serious is myocarditis and when should I seek specialist paediatric cardiology care in London?
Myocarditis is a serious cardiac condition requiring prompt specialist recognition and treatment. Severity ranges from mild disease with complete recovery to critical illness requiring intensive care. It remains a recognised cause of sudden cardiac death in children and young athletes, which is why proper assessment and treatment are essential. With appropriate management, most children achieve complete recovery.
Can myocarditis symptoms be mistaken for other childhood illnesses?
Yes, myocarditis is frequently initially misdiagnosed because symptoms mimic common childhood illnesses. Children are often thought to have respiratory illnesses like asthma or pneumonia, gastrointestinal problems, or simple flu. Many experience a preceding viral illness, making it difficult to recognise when infection has affected the heart. This is why evaluation by a paediatric cardiologist is important when cardiac symptoms are present, particularly after viral illness or when symptoms seem disproportionate to the apparent cause. Specialist assessment can perform comprehensive cardiac investigations to either confirm myocarditis and initiate treatment, or provide reassurance that the heart is functioning normally.
Will my child fully recover from myocarditis?
Many children achieve complete recovery. About two-thirds will have full recovery of heart function with appropriate treatment, typically within two to three months. However, some develop chronic myocarditis with ongoing mild inflammation, or have residual heart dysfunction from scarring requiring long-term follow-up. Regular monitoring with echocardiograms tracks recovery, and your paediatric cardiologist can provide an individualised prognosis based on the severity of the initial illness and how well the heart responds to treatment.
When can my child return to sports and physical activities after myocarditis?
This must be determined by your paediatric cardiologist based on your child’s specific cardiac function and recovery. Physical activity is typically restricted for several weeks to allow the heart to heal, with the restriction period depending on illness severity and recovery progress. Return to activity must be gradual and supervised, with clear guidance on when different activity levels are safe. Premature return to vigorous exercise can harm the healing heart. Your specialist will provide detailed guidance on activity restrictions and the timeline for safely resuming sports and physical activities.
What are the warning signs that my child’s myocarditis is worsening?
Warning signs requiring immediate medical attention include worsening shortness of breath, inability to lie flat due to breathing difficulty, severe chest pain, persistent palpitations, fainting or near-fainting episodes, extreme fatigue or lethargy, swelling of face or legs, reduced urine output, or any concerning change in condition. Children with myocarditis can deteriorate rapidly, so any worsening symptoms should prompt urgent reassessment at the emergency department or immediate contact with your paediatric cardiologist. Given the potential for rapid deterioration, it’s always better to seek urgent specialist assessment if there’s any concern about your child’s cardiac status.
Seeking Specialist Paediatric Cardiology Care for Myocarditis in London
If you’re concerned about myocarditis or other cardiac conditions in your child, Dr Alessandro Giardini is a Consultant Paediatric and Adolescent Cardiologist based in London with specialist expertise in myocarditis, congenital heart disease, hypertrophic cardiomyopathy, and inherited cardiac conditions in children and young people. Dr Giardini practices at Great Ormond Street Hospital and The Portland Hospital in London, providing expert paediatric cardiology care for families throughout London and the South East.