Brugada Syndrome in Children: A Guide for Parents
By Dr Alessandro Giardini, Senior Consultant Paediatric and Adolescent Cardiologist, Great Ormond Street Hospital, London
Hearing that your child may have Brugada syndrome, whether it has come up after an episode of fainting, an unexpected ECG finding, or a family history of sudden cardiac death, is naturally unsettling. The name alone can sound alarming, and the questions that follow tend to come quickly.
The important thing to understand from the outset is that Brugada syndrome is rare, and in most children the overall risk is low when the condition is properly assessed and managed. With thorough specialist evaluation, clear practical guidance, and appropriate follow-up, families can feel both informed and reassured. Dr Giardini regularly assesses children with fainting, abnormal ECGs, and inherited heart rhythm conditions across his private practice in London, providing families with clear answers and a coherent plan.
Key Facts About Brugada Syndrome in Children
Brugada syndrome affects the heart’s electrical system, and the heart muscle itself is structurally normal. Many children with the condition have no symptoms at all. It is most commonly identified on an electrocardiogram (ECG), and it is often inherited, making family screening an important part of care. Fever can provoke ECG changes and rhythm disturbances and should be treated promptly. Most children are at low risk, and specialist assessment is the key to identifying the small group who need additional protection.
What is Brugada Syndrome?
Brugada syndrome is a condition that affects the electrical activity of the heart rather than its structure. This distinguishes it from most other cardiac conditions discussed on this website: in Brugada syndrome, the heart looks entirely normal on an echocardiogram, and it is the way electrical signals travel through the heart cells that is abnormal.
These electrical signals control the rhythm of each heartbeat. In Brugada syndrome, under certain circumstances, most notably during fever or following exposure to particular medications, they can become unstable, creating conditions in which a dangerous ventricular arrhythmia could arise. In the great majority of children, however, the condition remains entirely silent and is discovered only when an ECG is performed for another reason, or when a family member is being screened.
What Causes Brugada Syndrome?
Brugada syndrome is in most cases a genetic condition. The gene most frequently implicated is SCN5A, which encodes a sodium channel protein in heart muscle cells. When this channel does not function normally, the pattern of electrical recovery across the heart is disrupted in a characteristic way that is visible on the ECG.
The condition is typically inherited in an autosomal dominant pattern, meaning that one copy of the altered gene is sufficient to cause the condition and that a parent may also carry it. Each sibling of an affected child has a one in two chance of having inherited the same variant. Family screening is therefore an important and practical part of management from the outset.
It is worth noting that not every child with Brugada syndrome has an identifiable genetic variant. In a significant proportion of cases, no causative change is found despite thorough genetic testing. In these children, the diagnosis rests on the ECG findings interpreted in clinical context, and the absence of a genetic result does not alter the need for careful monitoring.
What Are the Symptoms of Brugada Syndrome in Children?
One of the most clinically important features of Brugada syndrome is that many children who carry it never develop any symptoms. The condition may remain entirely quiescent throughout childhood and be identified only through screening or incidentally.
When symptoms do occur, they most commonly include fainting (syncope), characteristically at rest, during sleep, or in association with fever rather than during vigorous exercise, as well as palpitations, dizziness, and occasionally seizure-like episodes. The latter can be particularly misleading: the loss of consciousness and convulsive movements that accompany a ventricular arrhythmia in Brugada syndrome can be indistinguishable clinically from an epileptic seizure, and a cardiac cause is not always considered initially. Any child with unexplained seizure-like events, particularly during fever or at rest, warrants a careful cardiac assessment.
Unexplained fainting during a febrile illness is a specific warning sign in Brugada syndrome and should always prompt specialist review.
Why Does Fever Matter in Brugada Syndrome?
Fever occupies a uniquely important position in Brugada syndrome management, and parents need to understand why.
An elevated body temperature directly affects the function of the sodium channels that are already impaired in this condition. Even a moderate fever can unmask or intensify the characteristic ECG changes of Brugada syndrome and can increase the likelihood of a dangerous rhythm disturbance occurring. This is not a reason for alarm, but it is a reason for action. Fever in a child with known or suspected Brugada syndrome should be treated promptly with paracetamol or ibuprofen to bring the temperature down, and medical advice should be sought without delay if any symptoms develop alongside the fever.
The practical guidance is straightforward: treat fever early and act quickly if symptoms occur. This is one of the most tangible and effective protective measures available for children with this condition.
How is Brugada Syndrome Diagnosed?
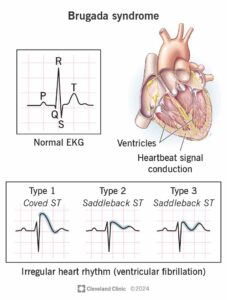
The electrocardiogram is the central diagnostic tool in Brugada syndrome. The condition produces a characteristic pattern, specifically a coved-type ST segment elevation in the right precordial leads, that is highly specific when correctly identified. However, this pattern is not always present on a standard resting ECG; it can be intermittent, subtle, or concealed, which is why experienced interpretation by a paediatric cardiologist matters greatly.
Where the resting ECG is not conclusive, further approaches are available. Repeat ECGs, particularly during a febrile illness or with modified lead positioning, can bring out changes not visible at other times. A pharmacological provocation test, in which a sodium channel blocking drug (like Ajmaline) is administered in a controlled specialist setting, can unmask the characteristic pattern in children where the diagnosis is suspected but not confirmed on the standard recording. This test is performed with appropriate monitoring and safety precautions.
Genetic testing for SCN5A and related genes is offered as part of the assessment. A positive result supports the diagnosis and, critically, enables precise cascade screening of family members. A negative result does not exclude the condition, and clinical evaluation of relatives remains important regardless.
Dr Giardini takes a systematic and thorough approach to the assessment of children with suspected Brugada syndrome, combining the ECG findings, clinical history, family history, and genetic results to arrive at an accurate and individualised diagnosis.
What is the Risk to My Child?
This is, understandably, the question that matters most to parents, and it deserves a clear and honest answer.
The reassuring reality is that the majority of children with Brugada syndrome are at low risk of serious events, particularly those who have no symptoms, no high-risk features on their ECG, and no family history of sudden cardiac death at a young age. For this group, careful monitoring and clear practical guidance, particularly around fever management and medication avoidance, constitute appropriate and effective management.
A smaller number of children have features that place them in a higher-risk category. These include a prior episode of ventricular arrhythmia or aborted cardiac arrest, a spontaneously abnormal ECG pattern as opposed to one that is only unmasked by provocation, and a relevant family history. Identifying this group accurately, and taking appropriate protective steps, is one of the most important functions of specialist care.
How is Brugada Syndrome Managed?
Management in Brugada syndrome is tailored carefully to the individual child and their risk profile.
Regular monitoring. Most children are followed up at regular intervals, with periodic ECGs and clinical review to track any changes in the ECG pattern or clinical status over time. The frequency of review is adjusted to the child’s individual risk.
Fever management. Prompt treatment of fever with paracetamol or ibuprofen is one of the most practically important protective measures, and families are given clear written guidance on this from the outset of care.
Medication awareness. A range of medications, including certain anaesthetic agents, antiarrhythmic drugs, psychotropic medications, and some common antibiotics, can provoke or worsen the Brugada ECG pattern and should be avoided. Dr Giardini provides families with clear guidance and advises that all healthcare professionals involved in the child’s care are made aware of the diagnosis. A reference list of drugs to avoid is available at brugadadrugs.org.
ICD implantation. In a small number of children identified as being at higher risk of life-threatening arrhythmia, implantation of an ICD may be recommended. This is not a common recommendation in the paediatric population, as most children with Brugada syndrome do not require a device, but it is an important option for those in whom the risk assessment supports it, and the decision is always made with careful discussion and full involvement of the family.
When Should I Seek Urgent Medical Advice?
The following situations in a child with known or suspected Brugada syndrome should prompt medical assessment: fainting or collapse during a febrile illness, collapse without warning or clear cause, episodes that resemble seizures, a family history of sudden unexplained cardiac death in a young person, and an abnormal ECG pattern found in a child or young adult.
None of these scenarios automatically implies a serious or imminent problem, but each warrants careful cardiac evaluation rather than a wait-and-see approach.
Frequently Asked Questions
Is Brugada syndrome dangerous in children?
For most children, the risk is low, and careful specialist assessment is the key to understanding where any individual child sits on that risk spectrum. The majority of children with Brugada syndrome live normal lives without any serious cardiac events. A smaller group has features that require more active management, and identifying them is precisely what specialist evaluation achieves.
Can a child with Brugada syndrome play sport?
Most children with Brugada syndrome can participate in normal physical activity, including school sport. Unlike some other inherited cardiac conditions such as hypertrophic cardiomyopathy or ARVC, exercise is not the primary trigger for arrhythmia in Brugada syndrome. Individual guidance is provided by Dr Giardini at clinic, taking into account the child’s specific risk profile.
Should siblings and parents be tested?
Yes. Because Brugada syndrome is usually inherited, all first-degree relatives, including parents and siblings, should be offered clinical evaluation including an ECG, and genetic testing where a causative variant has been identified in the affected child.
Does my child need genetic testing?
Genetic testing is a useful and recommended part of the assessment in most cases. However, it is not always definitive, and a negative result does not exclude the condition. The diagnosis rests primarily on ECG findings interpreted in clinical context. The main practical value of a positive genetic result is enabling accurate and efficient screening of family members.
Can fever trigger dangerous heart rhythms in my child?
In children with Brugada syndrome, fever can increase the risk of arrhythmia by worsening the underlying sodium channel impairment. This is why prompt fever treatment is so important. It is not a reason to live in fear of every childhood illness, but it is a reason to act quickly and to have paracetamol readily available.
What is a drug challenge test, and is it safe?
A drug challenge test, most commonly using ajmaline or flecainide administered intravenously, is used to provoke the Brugada ECG pattern in children where the diagnosis is suspected but not confirmed on a standard resting ECG. It is performed in a specialist cardiology setting with continuous ECG monitoring and full resuscitation facilities available. In experienced hands it is a safe and well-established diagnostic procedure, and Dr Giardini discusses its role and any relevant considerations fully with families beforehand.
Will my child always need to be under a cardiologist?
Yes, lifelong specialist cardiac follow-up is recommended for individuals with confirmed Brugada syndrome. The intensity of monitoring varies with risk, and many children require only annual review once their risk profile is established. Planning the transition from paediatric to adult cardiology care is an important component of long-term management, and one that Dr Giardini addresses with families well before that transition is due.
Specialist Brugada Syndrome Assessment in London
If you have concerns about your child’s symptoms, an abnormal ECG finding, or a family history of inherited heart rhythm conditions, early specialist assessment provides the clarity and practical guidance that families need. Families are welcome to self-refer, or to arrange a referral through their GP or paediatrician.
Dr. Alessandro Giardini, MD, PhD
Written 03/04/2026