Fainting and Syncope in Children and Teenagers
Watching your child collapse and lose consciousness is one of the most frightening experiences a parent can go through. Whether it happened at school, on the sports field, or simply standing up too quickly at home, the memory tends to linger long after your child has recovered and is back to normal. The reassuring news is that fainting (or syncope, as doctors call it) is extremely common in children and teenagers, and the majority of cases have a straightforward, benign explanation. Understanding what causes it, what to look out for, and when a specialist opinion is needed can make an enormous difference to how families cope.
This page has been written by Dr. Alessandro Giardini to help parents and young people navigate the subject clearly and confidently, drawing on current clinical evidence and the kind of questions that come up most frequently in the paediatric cardiology clinic.
What Is Syncope?
Syncope is the medical term for a temporary loss of consciousness caused by a brief reduction in blood flow to the brain. It comes on suddenly, causes the person to go limp and fall if they are not supported, and typically resolves within seconds to a minute or two. Recovery is usually rapid and complete, though many children feel tired, pale, or slightly nauseous afterwards.
It is important to understand that syncope is not the same as a seizure, a stroke, or a prolonged blackout. True syncope is brief, self-limiting, and leaves no lasting effects. That said, any episode of loss of consciousness in a child deserves proper evaluation, not because it is likely to be serious, but because a careful assessment allows the right reassurance to be given, and ensures the rare cases that do need treatment are not missed.
Fainting is remarkably prevalent in young people. Around 15 to 20 per cent of children and adolescents will experience at least one episode before the end of their teenage years, and the peak age is around 15, particularly in girls. In fact, for most teenagers a faint is a one-off event that never recurs.
What Causes Fainting in Children and Teenagers?
Vasovagal (Neurally Mediated) Syncope — The Simple Faint
By far the most common cause of fainting in children and teenagers is what doctors call vasovagal syncope, also known as neurally mediated syncope or, simply, the common faint. It accounts for between 60 and 80 per cent of all syncope in the paediatric age group.
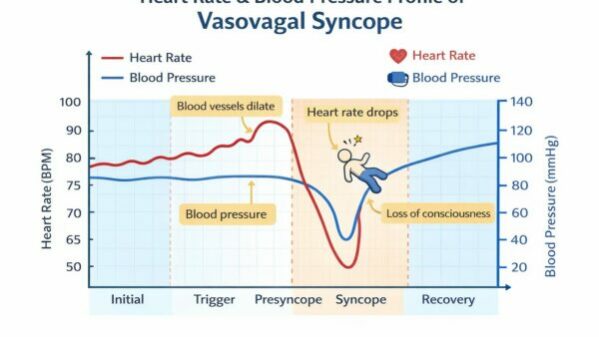
What happens in a vasovagal faint is that the body’s autonomic nervous system (the part that controls heart rate and blood pressure automatically) overreacts to a trigger. Blood pools in the legs, blood pressure drops, heart rate slows, and momentarily the brain does not receive enough blood to maintain consciousness. The whole process is self-correcting: once the child is horizontal, blood flow to the brain is restored and they wake up.
Common triggers include prolonged standing (in queues, assemblies, or hot classrooms), getting up too quickly, heat, dehydration, hunger, pain, emotional distress, or the sight of blood or needles. In adolescent girls, fainting can also be associated with growth spurts, menstrual cycles, and periods of rapid weight change.
The classic sequence is well recognised: the child notices they feel light-headed, nauseated, or hot; their vision may tunnel or go grey; they may look pale and sweaty. Then they faint. This warning phase, called the prodrome, is an important feature and, when present, is reassuring that the faint is benign in nature.
Orthostatic Intolerance and POTS
A related group of conditions involves difficulty maintaining blood pressure and heart rate when moving from lying or sitting to standing. The most discussed of these in teenagers is Postural Orthostatic Tachycardia Syndrome, or POTS. This is a condition where the heart rate rises abnormally on standing, causing dizziness, fatigue, brain fog, and sometimes fainting. POTS is more common in adolescent girls and can be associated with periods of rapid growth, prolonged periods of rest following illness, and occasionally anxiety.
POTS is not dangerous, but it can significantly affect quality of life, and it is very much manageable with the right approach. Increased fluid and salt intake, graded exercise, and in some cases medication can make a substantial difference.
Situational Syncope
Some children faint in very specific circumstances like during coughing, breath-holding, hair-brushing, urination, or swallowing. These situational faints follow the same basic mechanism as vasovagal syncope and are generally benign, though they can be alarming to witness.
Cardiac Syncope — The Important Minority
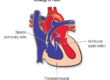
A small but important minority of fainting episodes in children have a cardiac cause. These are the cases that a paediatric cardiologist is specifically trained to identify. Cardiac syncope occurs when the heart’s output suddenly drops either because of an abnormal heart rhythm (arrhythmia), a structural problem such as hypertrophic cardiomyopathy or a congenital heart defect, or occasionally an abnormality of the heart’s electrical conduction system such as Long QT Syndrome or Wolff-Parkinson-White Syndrome.
The features that raise concern for a cardiac cause include syncope that happens during exercise rather than after it, syncope with no warning at all (so-called “drop attacks”), associated chest pain or palpitations before the episode, a personal or family history of sudden cardiac death at a young age, or an abnormal examination or ECG. When any of these features are present, prompt specialist evaluation is essential.
Dr. Giardini sees children across a wide range of inherited cardiac conditions including hypertrophic cardiomyopathy and channelopathies such as Long QT Syndrome where syncope may be the first presenting symptom, and where accurate diagnosis is critical.
What Are the Warning Signs That Need Urgent Attention?
Most faints do not need emergency treatment, but the following features should always prompt rapid medical evaluation:
Syncope that occurs during physical exercise — not after it — is the most important red flag. Fainting during exertion can indicate a serious underlying heart condition and must be investigated without delay.
Other features that should prompt urgent assessment include: loss of consciousness with no prodromal warning at all; associated chest pain or racing heartbeat; a seizure occurring at the same time or shortly after the episode; more than two or three unexplained episodes; a family history of sudden unexplained death in a young relative; or any known heart condition in the child.
If your child collapses and does not regain consciousness quickly, or if they are unresponsive and not breathing normally, call 999 immediately.
How Is Syncope Investigated?
History and Examination
The single most important diagnostic tool in syncope is a detailed, careful history. A specialist will want to understand exactly what happened before, during, and after the episode: what the child was doing, how they felt beforehand, how long they were unconscious, and how quickly they recovered. Details about the family history are equally important.
Dr. Giardini’s approach in clinic is to take the time to build a full picture through conversation with both the child and their family, rather than relying on investigations alone. In many cases, the history alone points clearly to the diagnosis.
Electrocardiogram (ECG)
A resting ECG: a recording of the heart’s electrical activity — is usually the first investigation performed. It takes only a few minutes and is entirely painless. The ECG can detect certain rhythm abnormalities and conduction conditions such as Long QT Syndrome, Brugada Syndrome, or pre-excitation patterns that might predispose to dangerous arrhythmias.
Echocardiogram
An echocardiogram (an ultrasound of the heart) is arranged when there is concern about structural heart disease. It allows detailed assessment of the heart’s chambers, valves, and muscle, and can identify conditions such as hypertrophic cardiomyopathy or congenital defects that may cause syncope.
Ambulatory Heart Rhythm Monitoring
If the ECG is normal but there is concern about a possible rhythm disorder, a Holter monitor or event recorder may be used to capture the heart’s rhythm over a longer period, typically 24 to 48 hours, or even weeks in some cases. This is particularly useful when episodes are frequent enough to be likely to occur during the monitoring period.
Head-Up Tilt Table Test
For children with recurrent unexplained syncope where vasovagal syncope is suspected but not confirmed, a head-up tilt table test can reproduce the conditions that provoke fainting in a controlled, safe environment. The child or teenager is strapped to a tilting table and gradually moved from horizontal to upright, while heart rate and blood pressure are monitored continuously. This test is performed in specialist centres and helps clarify both the diagnosis and the specific mechanism of the faint.
Blood Tests and Additional Investigations
Routine blood tests are not routinely recommended in all children with syncope, but may be helpful in selected cases to look for anaemia, dehydration, or metabolic causes.
What Treatments Are Available?
Reassurance and Lifestyle Measures
For the majority of children with straightforward vasovagal syncope, the most important treatment is education and reassurance. Understanding what triggers the faint, recognising the warning symptoms, and knowing what to do when they appear is genuinely empowering, both for the young person and for their family.
Practical lifestyle measures make a significant difference: drinking at least 2.0-2.5 litres of fluid per day, increasing dietary salt intake, avoiding prolonged standing in hot environments, and learning to recognise and act on the early warning signs of a faint. When a child feels the prodrome coming on, lying flat or sitting with the head between the knees, and tensing the muscles of the legs and abdomen, can often abort the episode entirely.
For children and teenagers with POTS the management is more articulate and includes graded exercise, lifestyle changes at times medications.
Medication
Medication is reserved for cases where lifestyle measures have not provided sufficient control, or where syncope is very frequent or disabling. A range of medications can be used depending on the underlying mechanism, including agents that support blood pressure and heart rate regulation. These decisions are made on an individual basis and are reviewed carefully over time.
Cardiac Pacing
In a very small number of children with the most severe form of vasovagal syncope, where the heart slows to a prolonged standstill during an episode — a cardiac pacemaker may be considered. This applies only to a tiny minority and is never the first line of treatment.
Management of Underlying Cardiac Conditions
Where syncope is caused by an identifiable cardiac condition, treatment is directed at that condition specifically. This may involve antiarrhythmic medication, ablation procedures to correct abnormal electrical pathways, or in conditions such as hypertrophic cardiomyopathy careful monitoring and risk stratification. Dr. Giardini’s specialist work in these cardiac conditions means that families dealing with these diagnoses can access highly experienced, focused care.
Syncope in Teenagers: A Special Mention
The teenage years present a particular peak in syncope incidence, and it is worth acknowledging that fainting can have a real impact on a young person’s confidence, social life, and participation in school and sport. Teenagers who have fainted in public, in a classroom, at a concert, or on the sports field often feel embarrassed, anxious, and reluctant to be in situations where it might happen again.
Dr. Giardini’s consultations always include the young person directly in the conversation. Understanding their own condition, knowing their triggers, and having strategies to manage or prevent episodes can restore a sense of control. For many teenagers, clear reassurance that the heart is structurally normal and that the condition will not cause sudden death is, in itself, profoundly helpful.
Anxiety and syncope are closely intertwined in some young people. Anxiety can lower the threshold for vasovagal episodes, and the fear of fainting can itself become a significant source of anxiety. A joined-up approach that addresses both the physiological and emotional dimensions is often the most effective.
Frequently Asked Questions
Is fainting dangerous in children?
In the vast majority of cases, no. Most fainting episodes in children and teenagers are caused by the common vasovagal faint: a benign, self-limiting response that does not carry any risk of harm to the heart. The principal risk is injury from the fall itself. That said, a specialist assessment is always worthwhile after a first episode to make sure the small minority of cases with an underlying cardiac cause are not missed.
My child fainted at school. Do they need to see a cardiologist?
Not every faint requires a cardiology referral, but if there is any uncertainty about the cause, if the episode happened during exercise, if there was no warning beforehand, or if there is a relevant family history, a paediatric cardiologist should be involved.
Can anxiety cause fainting?
Yes. Emotional distress, anxiety, and fear are well-recognised triggers for vasovagal syncope. In some teenagers, psychological factors play a significant role in the frequency of episodes, and addressing anxiety, through talking therapies or, where appropriate, medication, can reduce the number of faints considerably.
What should I do if my child feels faint?
Help them lie flat immediately, raising their legs slightly if possible. This restores blood flow to the brain quickly and may abort the faint entirely. Avoid letting them sit up too quickly after the episode, and keep them horizontal until they feel fully recovered. Ensure they are well hydrated and, if they are in a hot or crowded environment, move them to a cooler, quieter space.
Will my child grow out of fainting?
Many children do. Vasovagal syncope often improves naturally as the autonomic nervous system matures, and the majority of teenagers who experience fainting episodes find that they become less frequent or stop altogether in early adulthood. In the meantime, management strategies can significantly reduce the impact on daily life.
What is POTS and how is it treated?
POTS (Postural Orthostatic Tachycardia Syndrome) is a form of dysautonomia where the heart rate rises abnormally on standing, causing dizziness, fatigue, and sometimes fainting. It is most common in teenage girls. Management focuses on increased fluid and salt intake, a structured exercise programme, and in some cases medication. POTS is not dangerous, and most young people improve significantly with appropriate treatment and support.
Does fainting mean my child has a heart problem?
Not usually. The vast majority of children who faint have perfectly normal hearts. However, because a small number of fainting episodes do reflect an underlying cardiac condition, and because distinguishing between the two requires clinical expertise, a careful assessment by a paediatric cardiologist is always the right step when there is any uncertainty.
Can children with known heart conditions faint?
Yes, and in this group, syncope always warrants prompt specialist evaluation. Children with congenital heart disease, hypertrophic cardiomyopathy, inherited rhythm conditions, or other cardiac diagnoses may faint for the same benign reasons as any other child but they may also faint because of their underlying condition, and the two possibilities need to be carefully separated. Dr. Giardini’s expertise across congenital heart disease, hypertrophic cardiomyopathy, and inherited cardiac conditions means that families in this situation can access focused, experienced assessment.
When should I call an ambulance?
Call 999 if your child does not regain consciousness promptly, if they are not breathing normally, if the episode occurs during exercise, if they have a seizure during or after the episode, or if you have any doubt at all about whether they have fully recovered. When in doubt, it is always right to seek immediate help.
A Note on Private Consultations
Dr. Giardini offers private paediatric cardiology consultations at different London locations. Appointments are available to families seeking a specialist second opinion, a first assessment of a new episode of syncope, or ongoing management of a known cardiac condition. Referrals from GPs and paediatricians are welcome, and self-referral is also possible.
Dr. Alessandro Giardini, MD, PhD
Written 31/03/2026