Written by Dr Alessandro Giardini, Senior Consultant Paediatric and Adolescent Cardiologist in London, UK
What Is a Ventricular Septal Defect?
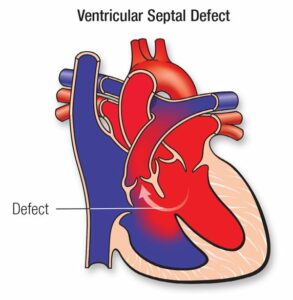
A ventricular septal defect — usually referred to as a VSD — is a hole in the wall (septum) that separates the two lower pumping chambers of the heart. It is the most common type of congenital heart defect, accounting for around 20 to 25 per cent of all heart conditions that babies are born with. Congenital heart defects themselves occur in roughly 8 out of every 1,000 live births, so VSDs are something that paediatric cardiologists see and manage very frequently.
To understand why a VSD matters, it helps to know how the normal heart works. The left side of the heart receives oxygen-rich blood from the lungs and pumps it out to the body. The right side receives oxygen-poor blood returning from the body and pumps it to the lungs to pick up fresh oxygen. The septum between the two lower chambers (ventricles) normally keeps these two circulations completely separate.
When there is a hole in the septum, blood is pushed from the left ventricle (where the pressure is higher) through the hole into the right ventricle and on to the lungs. This is called a left-to-right shunt. The result is that the lungs receive more blood than they should, and the left side of the heart has to work harder to keep up. Whether this causes any problems depends almost entirely on the size of the hole.
The reassuring reality is that many VSDs are small, cause no symptoms at all, and either close on their own or never need any treatment. As a paediatric cardiologist who sees children with VSDs on a daily basis, I find that the most important thing families need at the outset is a clear explanation of what kind of VSD their child has and what if anything needs to happen next.
What Causes a Ventricular Septal Defect?
In the vast majority of cases, there is no single identifiable cause. The heart forms during the first eight weeks of pregnancy, and the septum between the ventricles develops through a complex process in which several pieces of tissue grow together and fuse. If this process is not completed, a hole remains.
VSDs can occur as an isolated finding in an otherwise healthy baby, or they can be part of a broader pattern of heart defects. Occasionally, a VSD is associated with a genetic condition such as Down syndrome (trisomy 21) or other chromosomal abnormalities. In these cases, the VSD is usually identified as part of a wider assessment.
There is generally nothing that a parent did or did not do during pregnancy to cause a VSD. While certain factors — such as maternal diabetes, some medications, or heavy alcohol use — may slightly increase the overall risk of congenital heart defects, the overwhelming majority of VSDs occur without any identifiable risk factor.
What Are the Different Types of VSD?
VSDs are classified by their position in the ventricular septum, and the type of VSD your child has is important because it affects both the likelihood of spontaneous closure and the approach to treatment.
Perimembranous VSD
This is the most common type, accounting for about 80 per cent of all VSDs. The hole is located in the thin, membranous part of the septum near the top, close to where the heart valves sit. In some cases, tissue from the nearby tricuspid valve can partially cover the hole, forming a small pouch-like structure (sometimes called a ventricular septal aneurysm) that may help the defect get smaller or close altogether.
Muscular VSD
These holes sit within the thick, muscular part of the septum. They are relatively common in newborns and have the highest rate of spontaneous closure. Many will close within the first two years of life. Occasionally a child may have more than one muscular VSD.
Outlet (supracristal) VSD
This type is found high up in the septum, just below the pulmonary and aortic valves. It is less common overall but occurs more frequently in children of East Asian heritage. Outlet VSDs rarely close on their own and can sometimes cause the aortic valve to prolapse (sag) into the hole, which may lead to a leaking aortic valve over time.
Inlet VSD
These are located towards the back and bottom of the septum, near the tricuspid and mitral valves. They are often associated with a broader group of defects known as atrioventricular septal defects. Inlet VSDs do not tend to close spontaneously.
What Are the Symptoms?
Whether a VSD causes symptoms depends on the size of the hole and how much extra blood is being sent to the lungs.
Small VSDs typically cause no symptoms at all. The child grows normally, feeds well, and is otherwise completely healthy. The only clue may be a heart murmur which is an extra sound heard by a doctor when listening with a stethoscope. This is often how a small VSD is first discovered, either at a routine newborn check or at a later appointment.
Moderate to large VSDs send a significant amount of extra blood to the lungs. In babies, this typically becomes apparent in the first few weeks of life as the pressure in the lungs naturally drops after birth, allowing more blood to flow through the hole. Signs may include fast or heavy breathing, sweating during feeds, poor feeding and slow weight gain, and frequent chest infections. The baby may tire easily and may not be gaining weight as expected.
Very large, unrepaired VSDs, if left untreated over months to years, can eventually lead to permanently raised pressure in the lung blood vessels, a condition called pulmonary hypertension. In its most severe form (known as Eisenmenger syndrome), the lung pressures become so high that blood begins to flow the wrong way through the hole, from right to left, causing low oxygen levels. This is a serious, irreversible complication which is precisely why timely assessment and, when needed, early repair of large VSDs is so important.
How Is a VSD Diagnosed?
Echocardiogram (heart ultrasound)
This is the main tool for diagnosing and assessing a VSD. The echocardiogram shows the exact position, size, and number of holes, and allows the cardiologist to measure how much extra blood is crossing from left to right. It also shows whether the heart chambers have become enlarged as a result of the extra workload, and checks the function of nearby heart valves. Colour Doppler imaging — which shows the direction and speed of blood flow in colour — makes it straightforward to see the jet of blood passing through the defect. In my practice, the echocardiogram is the cornerstone of VSD assessment, and I always take time to show parents the images and explain what they mean.
Other tests
A chest X-ray may show an enlarged heart or increased blood flow to the lungs in cases of moderate or large VSDs. An electrocardiogram (ECG) records the electrical activity of the heart and can show signs of extra workload on the ventricles. In most cases, however, the echocardiogram provides all the information needed to make decisions about management.
Cardiac catheterisation is occasionally required, usually in older children or in cases where the lung pressures need to be measured accurately before a decision about surgery can be made. It is not needed for routine assessment of a straightforward VSD.
What Treatment Options Are Available?
The treatment of a VSD depends on the size and type of the defect, the symptoms it is causing, and whether it is affecting the heart or lungs. The approach ranges from simple observation through to surgery, and one of the most important parts of managing a VSD is knowing which category a child falls into.
Observation (watch and wait)
The majority of small VSDs and many moderate ones require no treatment other than regular follow-up with a paediatric cardiologist. Small muscular VSDs in particular have an excellent chance of closing on their own, most commonly by the age of two, though some continue to shrink throughout childhood. Small perimembranous VSDs may also get smaller, sometimes with the help of tricuspid valve tissue that partially covers the hole.
For children with small VSDs that remain open but cause no symptoms, follow-up can be quite relaxed with check-ups typically every one to three years, and in some cases the child can eventually be discharged from cardiology care altogether. I always explain to families at the outset what we are watching for and what would prompt us to change the plan.
Medical treatment
If a baby has a moderate to large VSD and is showing symptoms of heart failure (fast breathing, poor feeding, poor weight gain), medications can help manage these symptoms while the child grows. The most commonly used medicines are diuretics (such as furosemide), which help the body get rid of excess fluid and reduce the workload on the lungs, and sometimes digoxin, which helps the heart pump more efficiently. High-calorie feeding supplements or nasogastric tube feeding may be needed if a baby is not gaining weight adequately despite medication.
Medical treatment is not a cure for the VSD itself, it is a bridge used to support the baby either while waiting to see if the defect will get smaller, or while preparing for surgical repair.
Surgical closure
Surgery to close a VSD is recommended when the defect is large enough to cause significant symptoms, when it is not getting smaller on its own, or when there are signs that the extra blood flow is starting to affect the lungs or heart function. In general, elective surgical repair within the first one to two years of life is standard practice for large VSDs.
The operation is performed under general anaesthetic with the heart stopped temporarily using a heart-lung bypass machine. The surgeon opens the heart and closes the hole, usually with a small patch made from the pericardium (the natural lining around the outside of the heart). In some cases, very small holes can be closed with stitches alone. The heart’s own tissue grows over the patch in the weeks after surgery, making it a permanent part of the septum.
Surgical VSD closure is one of the most well-established operations in paediatric cardiac surgery. At experienced centres like the ones where I practice, the success rate is extremely high and the risk of serious complications is very low. Operative mortality is well under 1 per cent. Most children recover quickly, spending 1-3 days in intensive care followed by a short stay on the ward, and are usually home within a week.
The main risks of surgery include a small chance of damage to the heart’s electrical conduction system (which runs close to the septum), potentially requiring a permanent pacemaker. This complication occurs in fewer than 1 per cent of cases at the best centres. There is also a small chance of a residual leak around the patch, though this is usually minor and rarely needs further treatment.
Catheter-based (keyhole) closure
In some cases, a VSD can be closed without open-heart surgery, using a device delivered through a thin tube (catheter) inserted into a blood vessel in the groin and guided to the heart. A small umbrella-like device is positioned across the hole to seal it.
This approach works well for certain muscular VSDs that are away from the heart valves and conduction system. It is a less invasive option with a shorter recovery time. However, it is not suitable for all types of VSD. Perimembranous VSDs, the most common type, sit very close to the conduction tissue and the aortic valve, and catheter closure of perimembranous defects carries a higher risk of heart block. For this reason, surgical closure remains the standard approach for perimembranous VSDs in most centres.
Catheter-based closure should be performed at a centre with experience in this technique. I discuss all the available options with families so that together we can decide on the approach that is safest and most appropriate for each individual child.
Pulmonary artery banding
In certain complex situations — for example, in very small or premature babies who are too unwell for a full repair, or in babies with multiple VSDs, a temporary operation called a pulmonary artery band may be used. A band is placed around the main lung artery to restrict blood flow to the lungs, relieving the symptoms of heart failure and protecting the lung blood vessels while the baby grows. The band is removed at a later stage when the child is bigger and a full surgical repair can be safely performed.
This is a palliative (supportive) procedure rather than a definitive fix, and it is used much less commonly than direct surgical repair.
What Happens After Treatment?
After successful VSD closure, whether by surgery or catheter, the outlook for most children is excellent. The heart typically returns to a normal size, and children can expect to grow and develop normally with no restrictions on activity.
For children who have had a straightforward surgical repair with no residual leak and normal heart function, follow-up can be quite straightforward with usually a check-up every 2 to 3 years. If there is a small residual VSD or any concern about heart rhythm, valve function, or lung pressures, more frequent monitoring may be needed.
Children who had a small VSD that closed on its own may show a small outpouching on the septum where the hole was (a ventricular septal aneurysm). This is a normal finding and does not usually require any treatment but it is worth being aware of, because if it is seen on a future scan it can sometimes cause unnecessary worry if the context is not understood.
Frequently Asked Questions
My baby has been diagnosed with a VSD — does this always need surgery?
No. Many VSDs, particularly small ones, close on their own or remain small enough that they never cause any problems. Only moderate to large VSDs that cause symptoms, affect growth, or put strain on the heart and lungs will need to be closed. Your child’s cardiologist will monitor the VSD with regular echocardiograms and will recommend intervention only if it is genuinely needed.
When do most VSDs close on their own?
Small muscular VSDs have the best chance of spontaneous closure, and most close by the age of two. Some perimembranous VSDs also get smaller over time, occasionally closing completely by the age of four or five. Outlet and inlet VSDs, however, very rarely close on their own. Your cardiologist will be able to tell you what type of VSD your child has and what the chances of natural closure are.
How will I know if my baby’s VSD is causing problems?
The signs to watch for are fast or laboured breathing, sweating during feeds, poor feeding, slow weight gain, and frequent chest infections. Babies with large VSDs often tire quickly during feeds and may not finish a full bottle or breastfeed. If you are concerned, speak to your GP or contact your child’s paediatric cardiologist. In my experience, parents are often the first to notice that something is not right, and it is always better to check than to wait.
Is VSD surgery safe?
Yes. Surgical closure of a VSD is one of the most well-established operations in children’s heart surgery. At experienced centres like Great Ormond Street Hospital or The Portland Hospital, the risk of a serious complication is very low and operative mortality is well under 1 per cent. Most children recover quickly and are home within about a week. The long-term outlook after a successful repair is excellent, with the vast majority of children going on to lead completely normal lives.
Can a VSD be fixed without open-heart surgery?
In some cases, yes. Certain muscular VSDs that are positioned away from the heart valves and conduction system can be closed using a catheter-delivered device. This is a less invasive approach with a shorter recovery. However, the most common type of VSD (perimembranous) sits very close to important structures, and for these defects surgical closure remains the safest and most reliable option. I always discuss all the available approaches with families so that together we can choose the best option for their child.
Will my child need to take medication long-term?
In most cases, no. If medication (such as diuretics) is needed before surgery to manage symptoms of heart failure, it is usually stopped shortly after a successful repair. Most children who have had a VSD closed do not need any long-term medication. They also do not need antibiotics before dental procedures in most circumstances. This is a common misconception that has changed with updated guidelines.
Can my child play sport and be active after VSD repair?
Yes. Once the VSD has been successfully closed and the heart has returned to normal size and function, most children can take part in all physical activities without restriction. This is one of the most rewarding aspects of VSD repair as the vast majority of children go on to live completely normal, active lives. If there is any residual issue such as a small leak or a rhythm abnormality, your cardiologist will give specific guidance. As a specialist with a particular interest in exercise physiology in children with heart conditions, I am always happy to provide tailored advice on sport and activity.
Will the VSD come back after surgery?
It is very uncommon for a repaired VSD to reopen. Occasionally a tiny residual leak around the edge of the patch may be seen on follow-up scans, but this is usually insignificant and rarely needs further treatment. In the vast majority of cases, a single operation is all that is needed.
Does my baby need to see a cardiologist long-term after VSD closure?
Most children who have had a straightforward VSD repair will need periodic check-ups, typically every two to 3 years, to ensure everything remains well. These visits usually involve a clinical examination and an echocardiogram. Children whose VSD closed spontaneously and who have no murmur and a normal echocardiogram can often be discharged from routine follow-up. As part of my role at Great Ormond Street Hospital and in my private practice, I see children at all stages of the VSD journey, from first diagnosis through to long-term follow-up and I always aim to give families a clear plan for what lies ahead.
Where can I get specialist advice about my child’s VSD?
If your child has been diagnosed with a VSD and you would like a specialist assessment or a second opinion, I see children with all types of congenital heart disease including VSDs at my private clinics at The Portland Hospital, Chase Lodge, and Great Ormond Street Hospital, one of the world’s leading centres for paediatric cardiac care. You can find further information or get in touch through childheartspecialist.com.
Dr. Alessandro Giardini, MD, PhD
Written 29/03/2026