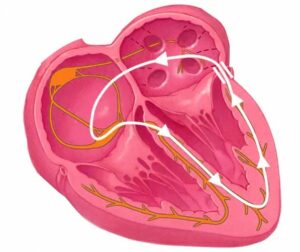
What Is Wolff-Parkinson-White Syndrome?
Wolff-Parkinson-White syndrome (WPW) is a heart condition caused by an extra electrical pathway in the heart. In a normal heart, electrical signals travel from the heart’s upper
chambers (the atria) to the lower chambers (the ventricles) through a single, carefully regulated route. In WPW, there is an additional, unregulated pathway — called an accessory
pathway or “bundle of Kent” — that can allow electrical signals to bypass the normal route and cause the heart to beat abnormally fast.
WPW affects approximately 1 to 3 in every 1,000 people and is one of the more common causes of heart rhythm problems (arrhythmia) in children and teenagers. It is present from birth, though many children have no symptoms whatsoever and the condition is discovered incidentally on a routine ECG — increasingly common as cardiac screening before sport becomes more widespread.
What Causes WPW?
WPW is caused by an abnormality in heart development before birth. In most cases it occurs with no family history and no identifiable cause. A small proportion of cases are hereditary, and WPW can occasionally be associated with other congenital heart conditions, most notably Ebstein’s anomaly, a malformation of the tricuspid valve. In the large majority of children, however, WPW occurs in an otherwise structurally normal heart.
What Are the Symptoms of WPW?
Many children and teenagers with WPW have no symptoms at all. The condition may be discovered entirely by chance when an ECG is performed for another reason — such as a
pre-sport medical, a school screening programme, or a routine paediatric check-up.
When symptoms do occur, the most common is a sudden episode of very fast heartbeat known as supraventricular tachycardia (SVT). During these episodes, the heart can race at 180–300 beats per minute. This typically feels like:
– A sudden, rapid fluttering or pounding in the chest
– Dizziness or light-headedness
– Feeling short of breath
– Chest discomfort or tightness
– Feeling faint, though actual loss of consciousness is uncommon
Episodes can start and stop suddenly, lasting seconds to hours. They can occur at rest, during exercise, or seemingly at random. In children, SVT episodes can be very frightening both for the child and for the parent witnessing them.
Rarely, WPW can be associated with a more serious arrhythmia — particularly a rapid, irregular rhythm called atrial fibrillation (AF) that in the context of an accessory pathway can occasionally lead to very fast ventricular rates. This is the basis for a small but real risk of sudden cardiac death in WPW, which is why the condition deserves careful evaluation.
How Is WPW Diagnosed?
– Electrocardiogram (ECG): The diagnosis of WPW is made on a standard 12-lead ECG. The accessory pathway produces a characteristic pattern, a “delta wave” (a slurred upstroke at the beginning of the QRS complex) and a shortened PR interval. An experienced Paediatric Cardiologist like Dr Giardini can identify this pattern at a glance.
– Holter monitor or event recorder: If a child has symptoms but a normal resting ECG, a longer-term heart rhythm monitor can help capture an episode and confirm the diagnosis.
– Echocardiogram: An ultrasound of the heart to check for any associated structural abnormality.
– Electrophysiology study (EPS): In children who are being considered for treatment, a more detailed test performed by passing fine catheters into the heart to map the electrical
pathways in detail. This is both diagnostic and the first step of curative treatment.
What Is the Risk of Sudden Cardiac Death in WPW?
This is understandably one of the first questions parents ask me when I see their children with WPW in my Paediatric Cardiology Clinics in London. The overall risk of sudden
cardiac death in WPW is low and is estimated at around 1 in 1,000 per year across the population of people with WPW. However, risk is not equal across all individuals.
Electrophysiological testing can identify features of the accessory pathway, specifically, how rapidly it can conduct electrical signals that stratify risk more precisely. Children with high-risk pathway features, or those with symptoms, are generally offered curative treatment.
It is also worth noting that WPW is one of the conditions that pre-sport cardiac screening is designed to detect. An ECG before competitive sport can identify WPW and allow risk
assessment before a child engages in vigorous athletic activity.
What Are the Treatment Options?
– No Treatment (Watchful Waiting)
Children who have been found incidentally to have a WPW pattern on ECG but have never had any symptoms require careful assessment. Many can be managed with observation, particularly younger children and those whose pathway is found to be low-risk on testing.
– Medications
Anti-arrhythmic medications can reduce the frequency of SVT episodes and are sometimes used as a short-term or bridging measure. However, they do not cure the condition.
– Catheter Ablation
This is the definitive and curative treatment for WPW. A cardiologist passes thin, flexible catheters through blood vessels into the heart and delivers precisely targeted
radiofrequency energy (or cryotherapy using extreme cold) to stun and destroy the accessory pathway. The procedure is performed under general anaesthetic in children and typically takes 2–4 hours. Success rates for catheter ablation in WPW are very high — around 95% or above in
experienced centres like the ones where Dr. Giardini practices. Most children go home the same day of the procedure and are back to normal activities within a week. Recurrence is possible but uncommon (approximately 5–8%), and a second procedure is highly effective if needed. Catheter ablation is generally recommended for children with symptomatic WPW, those with high-risk pathway features, and teenage athletes wishing to return to competitive sport without restriction.
Life After Treatment
Children who have had successful ablation can be discharged from cardiology follow-up and return to unrestricted physical activity, including competitive sport. Dr. Giardini offers his patients a follow up appointment after 3 months from the procedure and if there are no concerns children can be discharged from cardiologist follow up. For the many children with incidental, low-risk WPW who are managed conservatively, regular monitoring is recommended, particularly as they approach adolescence and may wish to take up competitive sport and Dr Giardini is very experienced in providing reassurance and advise in this setting.
Frequently Asked Questions:
Can WPW be present at birth with no symptoms until childhood or teenage years? Yes.WPW is a congenital condition present from before birth, but many people have no symptoms for years or decades. It is commonly first detected in childhood, teenage years, or even adulthood.
My child’s ECG showed a WPW pattern but they have never had symptoms. Do they need treatment? Not necessarily immediately, but I would recommend they do need careful assessment by a paediatric cardiologist like me. The decision about treatment depends on the characteristics of the accessory pathway, the child’s age, and their intended level of physical activity. I routinely guide my patients and their families trough this journey.
Is WPW hereditary? In most cases, WPW is not inherited. However, rare familial forms exist, and if one child has WPW, siblings may occasionally require screening. After a careful review I would be able to advise on the need based on your specific situation.
Can a child with WPW do sport? This depends on whether the WPW has been treated and the outcome of risk stratification. After successful ablation, most children can return to all sports including competitive athletics. Untreated symptomatic WPW or high-risk WPW generally requires restriction from intense competitive sport pending treatment or at least formal testing by a Paediatric Cardiologist.
Is catheter ablation safe in children? In experienced paediatric electrophysiology centres like Great Ormond Street Hospital or The Portland Hospital, catheter ablation is a well-established and safe procedure. As with all medical interventions there are small risks, which I will discuss in detail before any procedure. For children with symptomatic or high-risk WPW, the benefits of ablation significantly outweigh the risks.
What should I do if my child has a fast heartbeat episode? If your child has a known episode of SVT as is known to have WPW, vagal manoeuvres which can interrupt the arrhythmia should be used (such as bearing down or applying cold water to the face) to help terminate the
episode. If the episode lasts more than 15–20 minutes, causes significant symptoms, or your child is distressed, seek emergency medical assessment. If your child loses
consciousness, call 999 immediately. Dr. Alessandro Giardini provides in his London Paediatric Cardiology Clinics extensive training to the parents of children with WPW or supraventricular tachycardia so they can feel in charge and confident if their child has an episode of palpitation.
Does WPW affect daily life long-term? After successful ablation, most children have no long-term impact on their daily life whatsoever. Even those managed conservatively without ablation can often live normal lives with appropriate guidance and monitoring.
Dr Alessandro Giardini is a Senior Consultant Paediatric and Adolescent Cardiologist and offers Private Paediatric Cardiology appointments and testing to children with cardiac arrhythmias, SVT or WPW at Great Ormond Street Hospital and the the Portland Hospital with same day or next day appointments available. Week end appointments are also available.
Dr. Alessandro Giardini, MD, PhD
Consultant Paediatric Cardiologist
Written 25/03/2026